How Oura Smart Rings Are Shaping US Health Policy and Healthcare Legislation
The intersection of consumer health technology and government policy has become one of the most compelling narratives in modern healthcare. Over the past several years, a small Finnish company has quietly positioned itself at the center of this transformation. What began as a consumer wearable device has evolved into a tool that policymakers, legislators, and health officials are using to inform some of the most significant healthcare decisions being made in the United States today.
Oura, the company behind the distinctive smart ring that tracks everything from heart rate variability to sleep quality, has moved far beyond the fitness tracker market. The company's Chief Medical Officer and policy team have been actively engaged in conversations with some of the most influential figures in American politics and healthcare administration. From conversations with members of Congress to briefings with health-focused political figures, Oura is leveraging its technology and data insights to shape how the nation thinks about preventive health, health system economics, and the future of wearable medical devices.
The stakes of this engagement are genuinely high. The US healthcare system costs approximately $4.8 trillion annually, representing about 17.3% of GDP, yet Americans rank poorly on numerous health metrics compared to other developed nations. Preventive healthcare remains underfunded and underprioritized, with most of the healthcare budget dedicated to treating chronic diseases that could have been prevented or delayed. Smart ring technology represents a fundamentally different approach—continuous, non-intrusive health monitoring that could shift the entire healthcare paradigm from reactive treatment to proactive prevention.
What makes Oura's policy engagement particularly significant is the mounting evidence supporting wearable technology's effectiveness. Studies have shown that continuous biometric monitoring can detect health anomalies weeks or months before symptoms appear. A person's heart rate variability, for instance, can indicate immune system stress, cardiovascular health, and even mental well-being. Sleep quality metrics correlate strongly with cognitive performance, metabolic health, and longevity. When aggregated across millions of users, this data becomes extraordinarily valuable for understanding population health trends that traditional healthcare surveillance systems simply cannot capture.
Oura's vision extends beyond selling more rings. The company has articulated a long-term goal of fundamentally reshaping how health systems operate in the United States. This isn't merely about individual health optimization—it's about creating a new model where continuous preventive monitoring becomes the standard rather than the exception. The company's policy engagement reflects this ambition: they're not just trying to create a better product or expand their market share, they're attempting to influence the regulatory and legislative frameworks that will govern wearable health technology for decades to come.
This comprehensive guide explores how Oura is navigating the complex intersection of technology innovation and healthcare policy, the specific legislative initiatives they're influencing, the data and evidence supporting their policy positions, and what this means for the future of American healthcare. Whether you're a healthcare professional, policymaker, technology investor, or simply someone interested in the future of preventive medicine, understanding Oura's policy strategy provides crucial insights into how consumer technology is reshaping healthcare systems.
The Evolution of Oura: From Consumer Device to Policy Influencer
Origins and Market Development
Oura was founded in 2013 in Finland, emerging from a vision to create truly wearable biometric sensors. Unlike most early wearables that focused on step counting and basic activity tracking, Oura from its inception sought to measure more clinically meaningful metrics. The company developed proprietary algorithms to extract detailed health insights from signals that had been largely inaccessible to consumers—heart rate variability, skin temperature, respiratory rate changes, and sleeping heart rate patterns.
The initial Oura Ring launched in 2014 with a specific user base: quantified self enthusiasts and biohackers who wanted deep insights into their physiology. The device was positioned as a research tool as much as a consumer product. This origin story proved crucial. Unlike many consumer wearables that launched with flashy marketing focused on vanity metrics, Oura built its reputation on algorithmic sophistication and clinically relevant measurements. Early users were often software engineers, medical professionals, and serious health optimizers—people who understood and valued the complexity of the underlying science.
Throughout the late 2010s, Oura steadily improved its hardware and algorithms. The company published peer-reviewed research demonstrating the accuracy and utility of its measurements. Studies showed that Oura rings could detect illness before symptoms appeared, identify sleep disorders, and track cardiovascular health with clinical-grade accuracy. By 2019, the company had expanded to approximately 300,000 users worldwide. Importantly, these users tended to be relatively affluent, health-conscious, and embedded in professional networks that valued data-driven decision-making.
This demographic composition would prove strategically important. As Oura sought to engage with policymakers and legislators, its user base already included entrepreneurs, executives, investors, and professionals across multiple sectors. When legislative champions for health innovation emerged in Congress, many of them were simultaneously Oura users or had been introduced to the technology through their professional networks.
COVID-19: The Inflection Point for Health Monitoring
The COVID-19 pandemic fundamentally altered how both consumers and policymakers viewed continuous health monitoring. As the pandemic swept through the United States in 2020, healthcare systems became overwhelmed, and the limitations of reactive healthcare became starkly apparent. Suddenly, early disease detection wasn't just a luxury feature—it became a matter of life and death.
Oura experienced what many health technology companies experienced: explosive user growth. However, the company took a notably different approach than many of its competitors. Rather than simply scaling to meet demand, Oura systematically used the pandemic period to generate research evidence. The company partnered with multiple research institutions to study whether the Oura Ring could detect COVID-19 before symptoms appeared. The results were compelling: Oura-wearing participants showed detectable physiological changes an average of 1.5 days before symptom onset.
More significantly, Oura used the pandemic as an opportunity to engage with research scientists, epidemiologists, and public health experts. These relationships would later prove invaluable as the company began its policy engagement efforts. Researchers who had collaborated with Oura on COVID studies became advocates for the company's technology. They published findings in peer-reviewed journals, presented at conferences, and spoke to media about the potential of continuous biometric monitoring in public health contexts.
By 2022, as the acute phase of the pandemic subsided, Oura had transformed from a consumer gadget company into a research-backed health technology enterprise. The company had approximately 1 million users, published studies in prominent journals, and had established credibility with serious academics and medical professionals. This credibility would become the foundation for policy engagement.

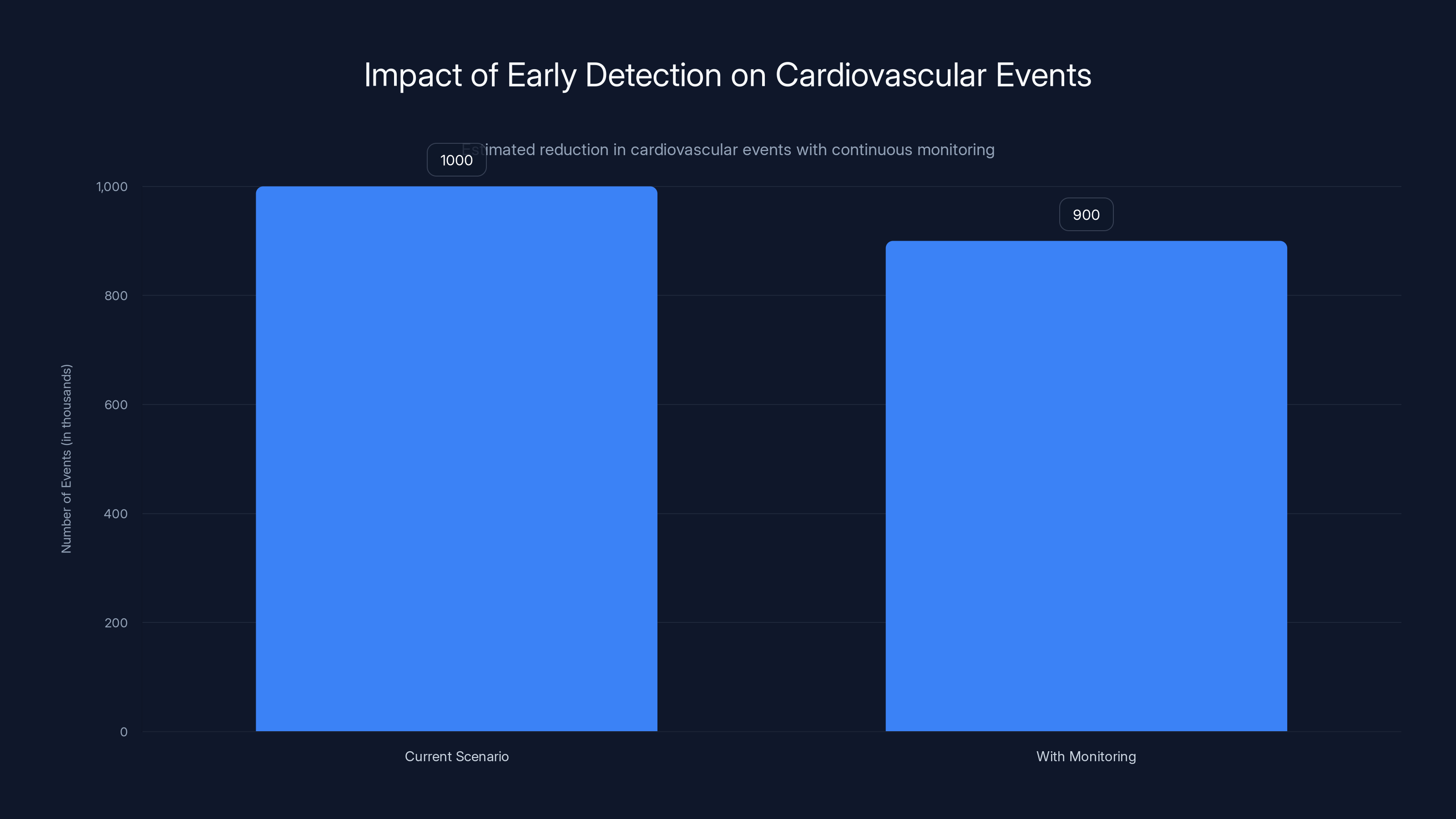
Estimated data suggests that if 5% of Americans used continuous health monitors, a 10% reduction in cardiovascular events could be achieved, significantly lowering healthcare costs.
Understanding Oura's Technology and Clinical Capabilities
The Science Behind the Measurements
To understand why Oura has become relevant in policy conversations, it's essential to understand what the technology actually measures and what that data reveals. Unlike fitness trackers that primarily count steps and estimate calories burned, Oura focuses on physiological parameters that have direct clinical significance.
Heart Rate Variability (HRV) represents the variation in time between successive heartbeats. While a completely regular heartbeat might seem optimal, the opposite is actually true. A healthy heart displays natural variation in its rhythm, responding to breathing patterns, emotional states, and nervous system activity. Higher HRV generally indicates better cardiovascular fitness and stress resilience. Lower HRV can signal illness, overtraining, poor sleep, or chronic stress. What makes HRV particularly valuable is that changes in HRV often precede symptomatic illness by days. A person might feel fine, but their HRV might drop by 20-30%, which often predicts that they'll develop cold symptoms within 24-48 hours.
Sleep metrics go far beyond simple duration measurements. Oura tracks sleep stages (light, deep, and REM sleep), sleep latency (how long it takes to fall asleep), and sleep efficiency (the percentage of time in bed actually spent sleeping). More importantly, the algorithms detect subtle changes in sleep architecture. When someone is developing an illness, their sleep changes before they're aware of being sick. Deep sleep and REM sleep ratios shift, awakenings increase, and sleep fragmentation becomes apparent. These changes are so consistent that researchers have used them as early illness markers.
Skin temperature fluctuations provide another layer of clinical insight. While absolute skin temperature varies based on environmental conditions, relative changes in skin temperature—particularly increases above a person's baseline—often indicate immune activation. During the early phases of infection, before fever develops systemically, skin temperature rises. This makes it an exceptionally sensitive marker for detecting illness in its earliest stages.
Respiratory rate is extracted from the ring's motion sensors. Elevated respiratory rate indicates cardiovascular stress, fever, anxiety, or physical exertion. Tracking how respiratory rate changes during sleep provides insights into sleep quality and respiratory health.
When these measurements are analyzed together, they create a comprehensive physiological profile. The algorithms Oura has developed analyze not just absolute values but, more importantly, deviations from individual baselines. This is crucial: every person has different baseline values. One person might have an HRV of 40 milliseconds while another has 120 milliseconds, and both might be perfectly healthy. By tracking how an individual's metrics change relative to their own baseline, the algorithms can detect meaningful changes that would be invisible in absolute value comparisons.
Clinical Accuracy and Validation
Oura's policy relevance partly stems from rigorous clinical validation. The company hasn't simply claimed its measurements are accurate—it has systematically published evidence demonstrating this accuracy in peer-reviewed journals. Multiple studies from respected research institutions have validated Oura's measurements against clinical gold standards.
For heart rate measurement accuracy, studies have shown that Oura's algorithms measure heart rate with error margins of ±1-2 beats per minute compared to electrocardiogram readings. For a consumer device, this represents clinical-grade accuracy. Sleep stage classification studies have shown accuracy rates of 85-90% when compared to polysomnography, which is the gold standard for sleep research.
Perhaps most importantly for policy discussions, Oura has published research demonstrating its capability to detect illness early. A study published in 2021 showed that machine learning models trained on Oura data could identify individuals with COVID-19 with sensitivity of 91.3% and specificity of 93.7% when the algorithm was applied to data collected before symptom onset. For policymakers concerned about pandemic preparedness, this level of predictive accuracy has massive implications.
Another study examining respiratory infection detection found that Oura metrics could identify 80% of respiratory infections 1.5 days before symptom onset. This early detection window is precisely what preventive healthcare systems need to function effectively. If you can identify illness before symptoms appear, you can isolate infected individuals faster, reduce transmission, enable early treatment, and prevent progression to severe disease.

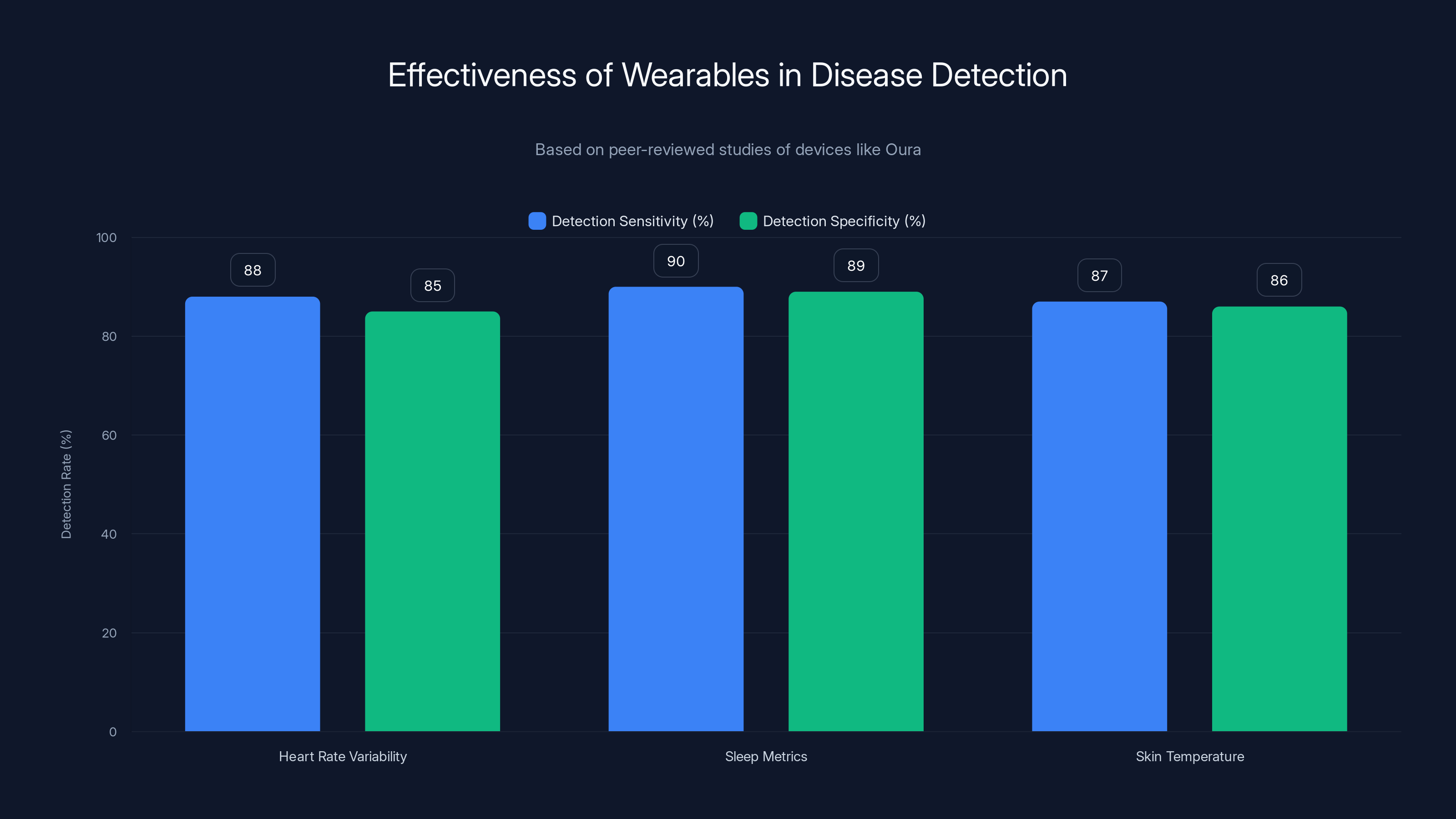
Wearables like Oura demonstrate high sensitivity and specificity in detecting diseases, with metrics such as heart rate variability and sleep patterns showing over 85% accuracy.
The Policy Engagement Strategy: How Oura Entered Healthcare Legislation Discussions
Building Relationships with Congressional Champions
Oura's entry into the policy sphere wasn't accidental—it followed a deliberate strategy. The company identified legislators and government officials who were already interested in health innovation and preventive medicine. These individuals often had existing relationships with venture capital firms investing in Oura, or they had encountered the technology through personal networks.
The initial engagement was exploratory. Oura executives and researchers conducted briefings with interested congressional staff members, presenting the clinical evidence for continuous biometric monitoring. These weren't sales pitches; they were technical presentations demonstrating what the technology could accomplish. Staff members reviewed published research, learned about the algorithms underlying the measurements, and understood the potential policy implications.
Key to Oura's approach was positioning the technology not as a consumer product but as a public health tool. Rather than focusing on individual health optimization, Oura framed the conversation around aggregated population health insights, early disease detection, and the potential to fundamentally shift healthcare economics by preventing disease rather than treating it.
The company also strategically engaged with thought leaders in healthcare policy who weren't confined to any single party or ideology. Oura's messaging resonated across the political spectrum in interesting ways: conservatives appreciated the emphasis on individual responsibility and market-driven innovation, while progressives saw potential for addressing health inequities through better data and earlier interventions.
Engagement with Diverse Political Figures
Oura's policy engagement has been notably bipartisan and ideologically diverse. The company has engaged with figures ranging from progressive Democrats focused on healthcare access and equity to health-focused figures in more conservative political movements. This diversity of engagement reflects both the fundamental appeal of preventive health technology and Oura's strategic approach to policy advocacy.
The company recognized that sustainable policy change requires building consensus across diverse constituencies. Rather than attempting to win on party lines, Oura identified shared values: the desire to improve health outcomes, the recognition that current healthcare systems are inefficient and expensive, and the potential of technology to solve some of healthcare's most intractable problems.
Engagement with various political figures has included providing data access to researchers in their networks, participating in policy roundtables, and educating stakeholders about wearable technology capabilities and limitations. Oura has been careful to position itself not as a lobbying force pushing a specific policy agenda, but as a resource providing technical expertise and evidence about what continuous health monitoring can accomplish.
The Public Health Case: Population-Level Evidence and Use Cases
Disease Detection and Early Intervention
When Oura engages policymakers, the conversation increasingly centers on population health benefits rather than individual consumer features. This reframing proves crucial for policy relevance. Policymakers care about aggregate outcomes: mortality rates, hospitalization rates, healthcare costs, quality-adjusted life years (QALYs), and disability-adjusted life years (DALYs).
The fundamental case Oura makes is elegant: continuous health monitoring enables early detection and intervention, which dramatically reduces disease progression and healthcare costs. Consider cardiovascular disease, the leading cause of death in the United States. Millions of Americans have undiagnosed hypertension or early-stage heart disease. By the time they're diagnosed, disease progression is often well advanced. However, heart rate variability and other metrics that Oura measures show changes in early disease stages.
Studies have established that heart rate variability strongly predicts cardiovascular mortality. Individuals with low HRV have significantly elevated risk of cardiac events. The mechanisms are understood: low HRV indicates dysfunction in the autonomic nervous system's ability to regulate cardiovascular function, suggesting underlying cardiac vulnerability. If continuous monitoring could identify individuals with declining HRV, clinical interventions (increased physical activity, stress reduction, dietary changes, or medications) could prevent disease progression.
Scaling this concept across a population becomes extraordinarily impactful. If even 5% of Americans wore continuous health monitors and early detection prevented just 10% of cardiovascular events, the reduction in mortality, morbidity, and healthcare costs would be staggering. A cardiovascular event costs the healthcare system approximately
Oura has extended this analysis to multiple disease categories. Type 2 diabetes represents another significant case. Blood glucose dysregulation often progresses silently for years before diagnosis. By the time someone is diagnosed with diabetes, beta cell dysfunction is already substantial. Yet sleep quality, heart rate patterns, and other metrics Oura measures correlate with glucose metabolism. Early interventions based on these signals might prevent progression from prediabetes to diabetes in a meaningful percentage of individuals.
Mental Health and Stress Detection
Another compelling area for policy engagement involves mental health and stress-related disorders. Depression and anxiety represent some of the largest causes of disability globally. Yet these conditions often go undiagnosed because they're invisible—a person looks fine externally while experiencing significant psychological distress.
Oura's metrics reveal signatures of mental health conditions. Heart rate variability decreases with anxiety and depression. Sleep becomes fragmented and restorative sleep decreases. Skin temperature patterns change. Respiratory rate becomes elevated during rest. These physiological markers appear before or alongside subjective awareness of mental health deterioration. For a segment of the population, wearable devices might serve as mental health canaries in the coal mine—objective markers that something is wrong and intervention is needed.
The policy appeal is significant. Mental health parity laws require insurance coverage for mental health treatment equivalent to physical health treatment, but mental health conditions remain dramatically underfunded and under-treated. Objective biomarkers for mental health conditions could potentially enable earlier diagnosis, more equitable treatment allocation, and better integration of mental and physical healthcare.
During policy briefings, Oura has presented research showing relationships between physiological metrics captured by the ring and validated mental health instruments like the PHQ-9 (for depression) and GAD-7 (for anxiety). While correlations don't establish causation, they suggest that wearable-derived metrics could serve as screening tools, flagging individuals who should undergo formal mental health evaluation.
Workplace Health and Productivity Economics
One area where Oura's policy engagement has gained traction involves workplace health and productivity. American employers face enormous costs from absenteeism, presenteeism (working while ill), and reduced productivity due to poor health. When employees are getting inadequate sleep, experiencing high stress, or developing illness, their productivity and creativity decline measurably.
Studies quantify these costs: a single case of the flu costs employers approximately
Oura has proposed that workplace wellness programs integrating continuous health monitoring could significantly reduce these costs. The model would involve employees wearing Oura rings, with data aggregated at a population level (protecting individual privacy) to understand workplace health trends. When health metrics deteriorate, employees would be encouraged to take preventive action—stay home if developing illness, access mental health resources, adjust workload and sleep patterns, etc.
For policymakers, the case is compelling: better workplace health translates to better productivity, reduced healthcare costs, and improved quality of life for workers. For employers, the business case is clear: preventing illness and managing health factors like sleep and stress creates significant economic value. This bipartisan consensus—benefiting workers, employers, healthcare systems, and government through reduced public health costs—has helped Oura's workplace health initiatives gain traction in policy discussions.

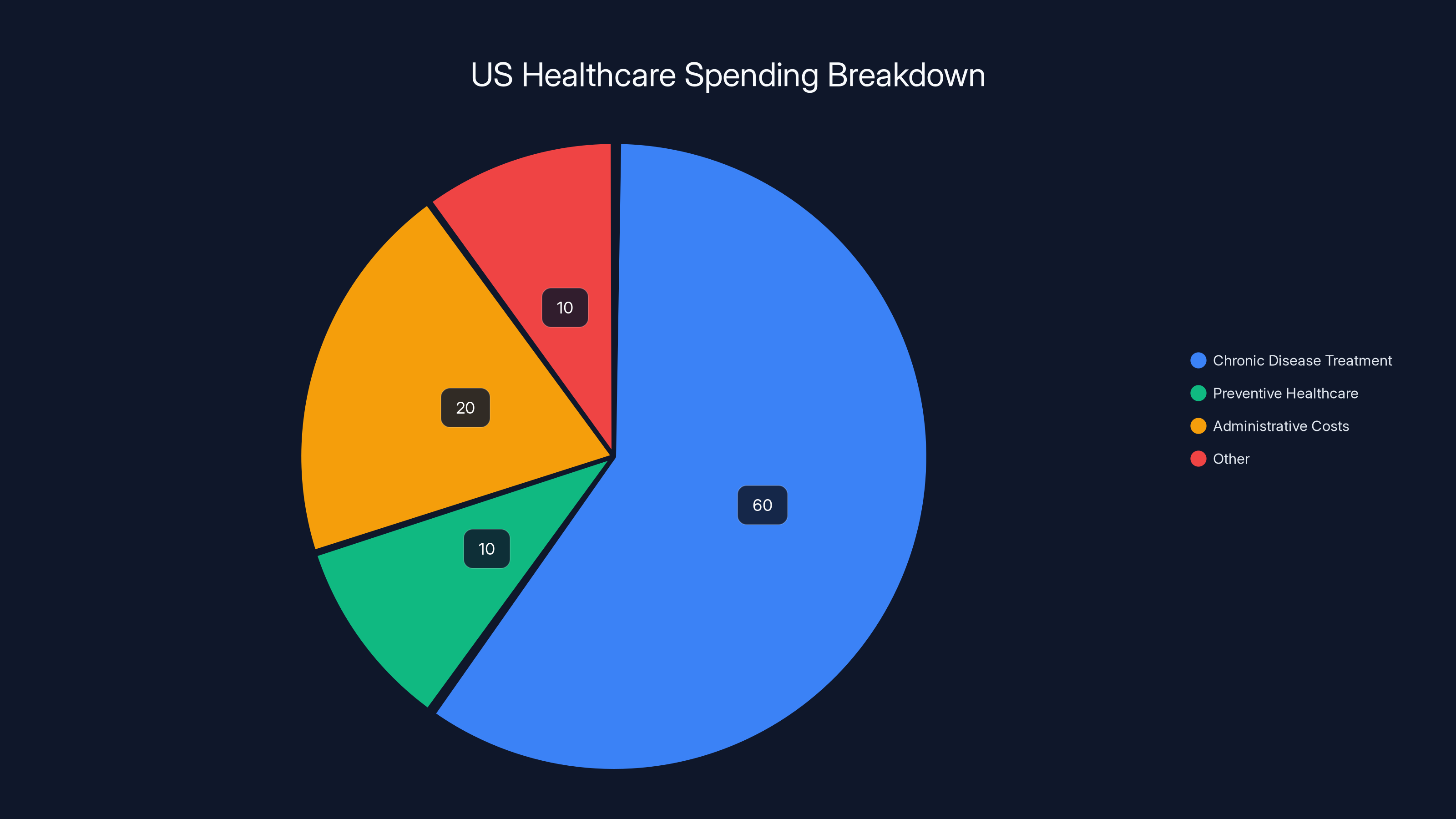
Chronic disease treatment dominates US healthcare spending, highlighting the potential impact of preventive technologies like Oura rings. Estimated data.
Regulatory Landscape: How Oura Navigates FDA and Healthcare Policy
Regulatory Classification and Compliance Strategy
Oura's policy engagement exists within a complex regulatory environment. The FDA classification of wearable devices determines what claims the company can make, what evidence must be provided, and what regulatory pathways are required. Understanding Oura's regulatory strategy illuminates how they approach policy engagement.
The FDA categorizes medical devices into three classes based on risk and required regulatory controls. A Class III device (highest risk, requiring premarket approval) requires enormous resources and evidence before commercialization. A Class II device (moderate risk, requiring 510(k) premarket notification) requires evidence of substantial equivalence to existing devices. A Class I device (lowest risk) requires only general controls.
Oura has strategically positioned its product in a regulatory gray zone. The ring itself isn't marketed as a medical device treating or diagnosing disease—it's marketed as a consumer wellness device. This allows the company to avoid the massive regulatory burdens of the Class II or III pathways. However, Oura simultaneously conducts research validating its measurements against clinical standards and demonstrating clinical utility.
This strategy creates space for policy engagement. Oura can sponsor research demonstrating clinical capabilities without those claims being regulatory violations. The company can publish evidence that their measurements predict disease outcomes without being required to seek FDA approval for a "disease prediction device." This regulatory positioning enables Oura to maintain the flexibility necessary for rapid innovation while building the evidence base policymakers need.
However, this regulatory strategy also creates tension. If Oura's evidence becomes sufficiently robust that the ring genuinely functions as a medical device, regulatory requirements might eventually change. Some policymakers are interested in clarifying the regulatory pathway for wearables more generally. Should devices demonstrating clinical utility be required to pursue formal approval? Should there be a new regulatory classification specifically for continuous monitoring devices that differ in fundamental ways from traditional diagnostic devices?
Oura's policy engagement includes conversations about how regulation should evolve. The company advocates for regulatory pathways that ensure safety and efficacy (protecting consumers) while enabling innovation and market entry (fostering competition). This balanced approach resonates with policymakers across the spectrum who recognize that over-regulation stifles innovation while under-regulation risks consumer harm.
Data Privacy and Security Policy
Another crucial policy domain involves data privacy and security. Continuous health monitoring generates enormous amounts of sensitive personal data. Healthcare data breaches have become increasingly common and costly. Consumer trust in sharing health data with companies requires confidence that data will be protected.
Oura has engaged with policymakers on data governance frameworks. The company supports strong privacy protections while arguing for responsible data use. This involves several policy dimensions:
Individual Privacy Protection: Oura advocates for policies ensuring individuals own their health data, can control how it's used, and have right to deletion. The company supports standards that let users port data between platforms and maintain transparency about data use.
Aggregate Research Use: Simultaneously, Oura supports policies enabling aggregated, de-identified health data to be used for research that advances public health. Large-scale studies examining how physiological patterns correlate with health outcomes require substantial datasets. Policies should enable this research while maintaining individual privacy.
Data Security Standards: Oura supports mandatory security standards for healthcare companies handling sensitive data. These include encryption, secure authentication, regular security audits, and breach notification requirements.
Equity and Access Considerations: Policy discussions increasingly address whether health data from wearables should be accessible to researchers studying health equity issues. Underrepresented groups in research have historically suffered when data collection doesn't include them. Wearable data offers opportunities for inclusive health research if privacy is protected while enabling research participation.
Oura's policy engagement on these issues positions the company as a responsible actor committed to both innovation and consumer protection—a positioning that strengthens relationships with policymakers who must balance multiple stakeholder interests.

The Clinical Evidence Foundation: What Research Shows
Published Studies and Academic Partnerships
Oura's policy credibility ultimately rests on research evidence. The company has systematically built an academic evidence base through partnerships with leading research institutions. These partnerships generate publications in peer-reviewed journals, the gold standard for scientific credibility.
Key published studies have demonstrated several critical capabilities:
Illness Detection Studies: Research published in multiple journals has shown that Oura metrics can detect respiratory infections, COVID-19, and other illnesses before symptom onset with sensitivity and specificity comparable to or exceeding many clinical diagnostic tests.
Sleep Quality and Health Outcomes: Studies have validated Oura's sleep measurements against polysomnography and demonstrated relationships between sleep metrics from the ring and health outcomes like cardiovascular health, metabolic function, and immune response.
Cardiovascular Health Monitoring: Research has shown that HRV measured by Oura correlates with clinical measures of cardiovascular function and predicts cardiovascular outcomes.
Stress and Recovery Tracking: Studies demonstrate that metrics captured by Oura correlate with physiological stress markers and recovery status, relevant for both individual health optimization and workplace wellness applications.
These publications matter enormously in policy contexts. When Oura's Chief Medical Officer briefs congressional staff, they can reference peer-reviewed research demonstrating the technology's capabilities. This differs fundamentally from marketing claims. A peer-reviewed study published in a respected journal with independent researchers vouching for methodology and results carries weight with evidence-conscious policymakers.
Real-World Effectiveness Research
Beyond clinical studies in research settings, Oura has increasingly sponsored research examining real-world effectiveness. Real-world evidence addresses questions that clinical trials can't: does this technology actually improve health outcomes when used by regular people outside research settings?
One notable study examined a large cohort of Oura users and investigated whether engaging with Oura's insights about sleep, activity, and stress improved health outcomes. Results showed that users who actively engaged with their data and made behavior changes experienced measurable improvements in sleep quality, reduced stress markers, and better self-reported health. This suggests that the technology works not just as a measurement system but as an effective health behavior change tool.
Another line of research examines health disparities. Preliminary data suggests that continuous monitoring might identify undiagnosed conditions in populations with limited healthcare access. If wearable technology could serve as a screening tool, identifying at-risk individuals who could then be connected to clinical care, it might reduce health disparities.
This real-world evidence is crucial for policy impact. Policymakers allocate resources based on demonstrated effectiveness. If research shows that wearable-based interventions actually improve population health outcomes and reduce healthcare costs, policymakers become far more inclined to support policies enabling broader adoption.

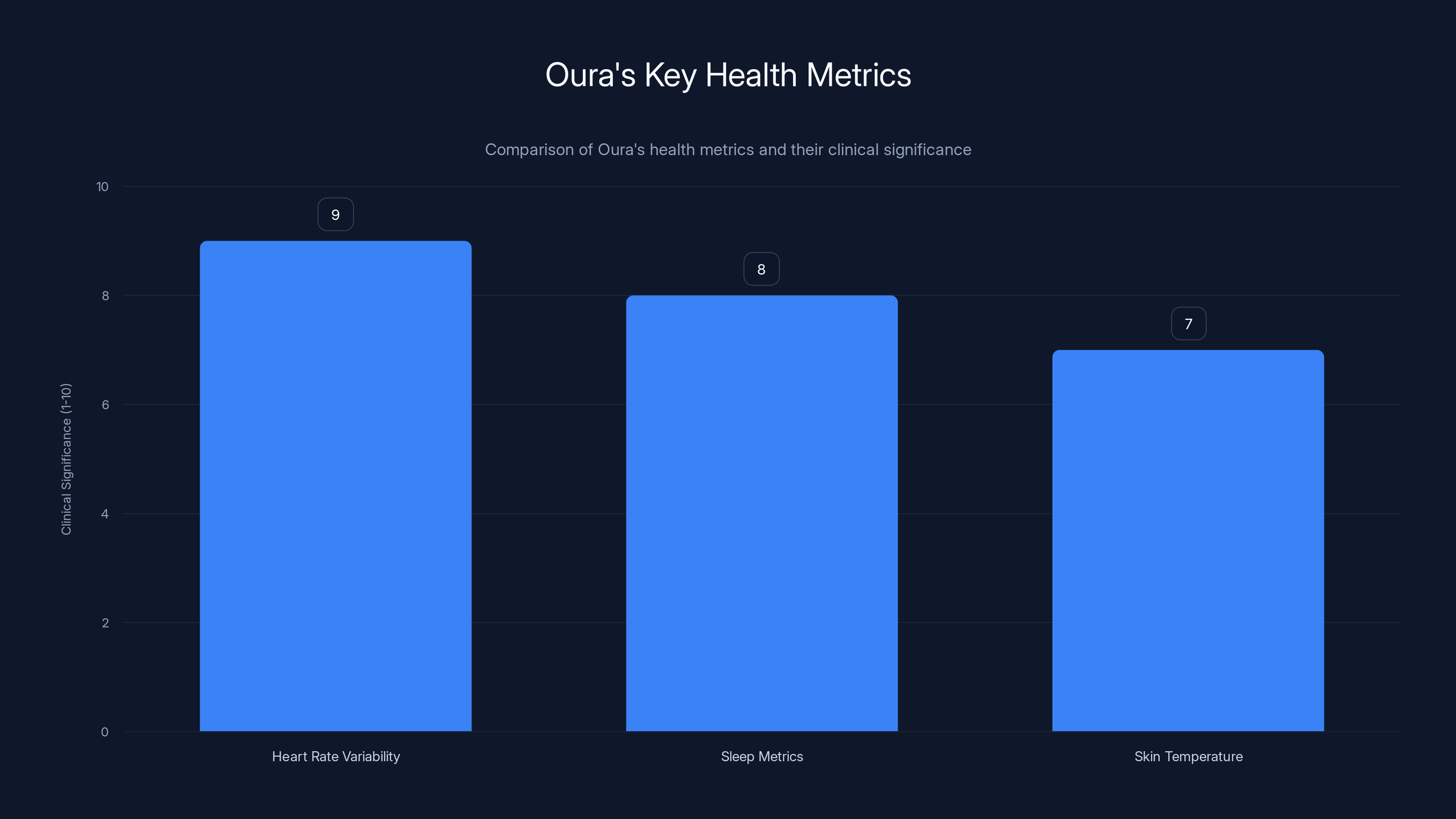
Oura's technology focuses on heart rate variability, sleep metrics, and skin temperature, each offering significant clinical insights. Estimated data based on typical clinical relevance.
Healthcare System Economics: The Cost-Benefit Case
Prevention vs. Treatment Economics
Underlying Oura's policy engagement is a fundamental economic argument: prevention is vastly more cost-effective than treatment. American healthcare spends approximately 97% of resources on treating disease and only 3% on prevention. Yet evidence overwhelmingly shows that preventing disease is far cheaper than treating it.
Consider type 2 diabetes. The United States spends approximately
Oura's argument is that continuous health monitoring enables the shift from treatment to prevention by identifying at-risk individuals early. This economic case resonates with policymakers managing constrained healthcare budgets. If wearable technology could shift healthcare toward prevention, the implications for healthcare costs and government budgets are enormous.
The company has engaged with policy analysts to model the economic impact of expanded wearable health monitoring. Preliminary analyses suggest that widespread adoption of continuous monitoring with clinical-grade accuracy could save the healthcare system
While these projections contain substantial uncertainty, they illustrate why policymakers take Oura's policy engagement seriously. If even a fraction of these savings materialize, the policy implications are profound.
Healthcare System Transformation Pathways
Oura's policy engagement increasingly focuses on how healthcare systems should adapt to leverage continuous monitoring. This involves discussing:
Integration with Electronic Health Records: For wearable data to be clinically useful, it needs integration with electronic health records. Policymakers are exploring standards enabling seamless data flow from wearable devices to clinical systems, ensuring that providers have access to relevant patient data when making clinical decisions.
Reimbursement Models: Current healthcare reimbursement doesn't adequately compensate providers for preventive care enabled by wearables. Policy discussions address how reimbursement should evolve to incentivize preventive care. Should providers be reimbursed for monitoring patients with wearables? How should risk-adjusted outcomes-based payment models be structured in an era of continuous health monitoring?
Care Delivery Models: Continuous monitoring requires new clinical workflows. Rather than annual checkups, providers might conduct more frequent remote interactions based on monitored health metrics. Policy discussions address how healthcare should be reorganized around continuous monitoring rather than episodic acute care.
Digital Health Infrastructure: Widespread adoption of health monitoring requires robust digital infrastructure. Policymakers are considering what investments in digital health capacity are needed, how healthcare systems should be funded to implement these technologies, and what standards enable interoperability.
These policy conversations extend beyond any single company's interests. They address fundamental questions about how healthcare systems should evolve in an era where continuous biometric monitoring is possible. However, Oura's policy engagement shapes these conversations by providing specific evidence about what continuous monitoring can accomplish and what barriers exist to broader implementation.

Public Health Applications: Population Health and Disease Surveillance
Early Warning Systems for Disease Outbreaks
One compelling area for policy impact involves using wearable data for disease surveillance. Public health agencies currently track disease outbreaks through clinic visits, lab reports, and hospital admissions. By the time an outbreak is identified through traditional surveillance, substantial transmission has already occurred.
Continuous monitoring offers an alternative: physiological markers suggesting illness appear days before diagnosis through traditional channels. If millions of people wore health monitoring devices, aggregated population-level patterns might detect disease outbreaks in real-time. This early detection could enable rapid public health response—identifying hotspots, implementing targeted interventions, and preventing spread.
Oura has engaged with public health officials about this potential. The company has demonstrated that they can detect trends in respiratory illness at the population level using aggregated, de-identified data from their user base. When respiratory illness surges in a geographic region, corresponding changes in Oura metrics appear days before traditional surveillance systems detect the surge.
For policymakers concerned about pandemic preparedness, this capability has significant appeal. The COVID-19 pandemic revealed weaknesses in traditional disease surveillance. By the time authorities recognized an outbreak, exponential spread was already underway. Wearable-based surveillance could enable much earlier detection.
Policy discussions address how such a system might work: What privacy protections are needed? How would data flow to public health agencies? What liability frameworks apply? How would equity be ensured, given that early adopters of wearables skew toward wealthier demographics? These nuanced policy questions don't have simple answers, but Oura's engagement is helping policymakers think through them.
Healthcare Access and Equity Considerations
Wearable health monitoring raises important equity questions. Current Oura users skew toward affluent, tech-savvy, health-conscious demographics. Without intentional policy efforts, wearable-based health improvements could exacerbate existing health inequities rather than reduce them.
Oura has engaged with policymakers on equity considerations. Policy proposals under discussion include:
Universal Access Programs: Should government make wearable devices accessible to underserved populations? Some policymakers propose subsidizing wearables for low-income individuals, similar to how Medicaid covers traditional healthcare.
Clinical Research Inclusion: Should health systems prioritize including underrepresented groups in clinical research using wearables? Historically, health research has underrepresented minorities and rural populations, leading to medical knowledge that's less applicable to these groups. Intentional research inclusion could correct this.
Data Sharing for Equity Research: Should de-identified wearable data be accessible to researchers studying health disparities? Large-scale data from diverse populations could enable understanding of how physiological patterns differ across demographic groups and inform more equitable healthcare approaches.
Healthcare System Integration: Should wearable data be integrated into primary care for underserved populations, potentially enabling early detection and intervention for individuals who otherwise have limited healthcare access? Some pilot programs are testing this model.
These equity-focused policy discussions are important because they address how transformative health technology gets distributed through society. Without intentional policy frameworks, transformative benefits accrue primarily to the already-advantaged.

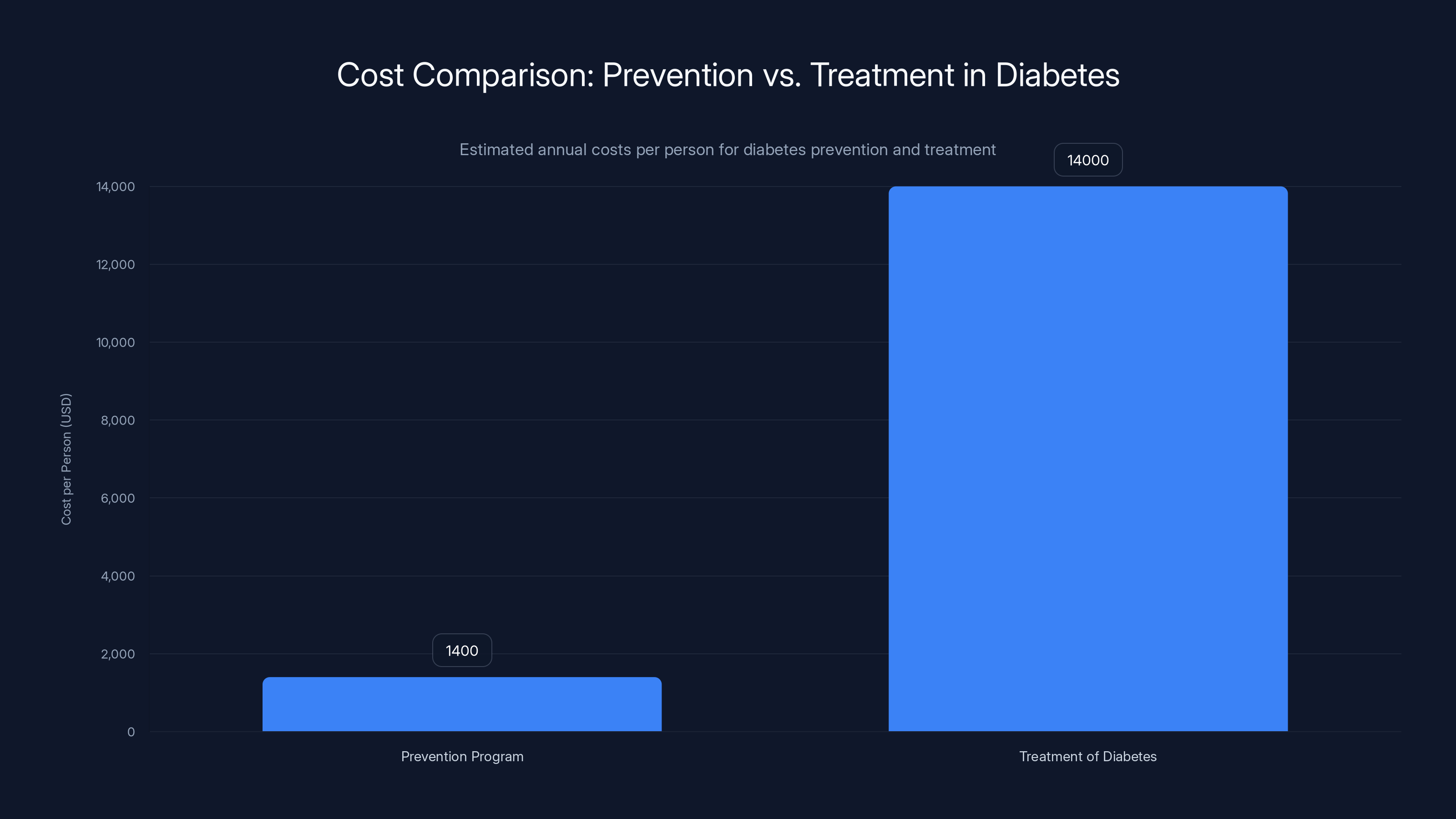
Prevention programs cost significantly less per person (
Comparative Analysis: Oura and Alternative Health Monitoring Approaches
Wearable Device Competitors and Differentiation
Oura doesn't operate in isolation. Multiple companies offer wearable health monitoring devices, each with different capabilities and market positions. Understanding how Oura's policy engagement compares to competitors' approaches illuminates what makes Oura's strategy distinctive.
Smartwatches from Tech Giants: Companies like Apple, Samsung, and Google have incorporated health monitoring into smartwatches. These devices measure heart rate, blood oxygen, activity, and increasingly sleep and stress metrics. They reach far larger user bases—tens of millions of users—compared to Oura's roughly 2-3 million users. However, smartwatches prioritize feature breadth and consumer appeal over specialized health measurement. They're excellent for general health awareness but less precise for clinical applications.
Dedicated Fitness Trackers: Companies like Fitbit, Garmin, and others offer devices focused on activity tracking, sleep, and health metrics. These have substantial user bases and measure many metrics Oura measures. However, they've traditionally prioritized consumer markets over clinical applications, and their policy engagement has been less systematic than Oura's.
Clinical-Grade Wearables: Some companies focus explicitly on clinical applications, partnering with hospitals and healthcare systems to monitor patients with chronic diseases. These devices often require prescriptions and insurance coverage but serve narrower populations with specific medical conditions.
Smartphone-Based Solutions: Companies like Runable offer various health automation and tracking capabilities integrated into software platforms, providing flexible health monitoring without specialized hardware.
Oura's distinctive positioning involves several factors:
Clinical Focus: While consumer-facing, Oura consistently emphasizes clinical rigor. The company publishes validation studies and frames discussions around health outcomes rather than consumer features. This positions Oura to engage with healthcare professionals and policymakers rather than just consumers.
Accuracy and Precision: The Oura Ring's design—worn on the finger close to arteries and capillaries—enables precise biometric measurement. The algorithms are highly optimized for the device's specific placement and sensors.
Privacy-First Data Approach: Oura maintains tight control over its data and is relatively restrictive about third-party access compared to some competitors. This positions the company as privacy-conscious in policy discussions.
Policy Engagement Strategy: Oura has systematically engaged with policymakers and researchers in ways some competitors haven't. The company invests in the relationships and evidence-building necessary for policy influence.
These differences matter for policy impact. Policymakers take Oura seriously partly because the company consistently shows up in policy spaces with credible evidence and sophisticated understanding of healthcare and policy issues.

The Specific Policy Initiatives: What Legislation Is Oura Influencing?
Wearable Health Technology Legislation
Oura's policy engagement has focused particularly on legislation creating frameworks for wearable health technology. Several legislative initiatives at federal and state levels aim to clarify how wearables should be regulated, how data should be governed, and how their use should be encouraged in clinical and public health contexts.
FDA Regulatory Reform: Legislation under discussion would establish a new regulatory pathway specifically for continuous monitoring devices. Traditional FDA pathways weren't designed for devices that measure multiple parameters, update algorithms based on new evidence, and serve both consumer and clinical purposes. Proposed reforms would create pathways acknowledging these differences while ensuring safety and efficacy. Oura has provided technical expertise informing these discussions.
Health Information Interoperability Standards: Legislation promoting the adoption of standards enabling wearable data to integrate with electronic health records. These standards are crucial for clinical utility—if providers can't access wearable data, they can't use it in clinical decision-making. Oura has engaged in standards discussions and endorsed proposed legislation.
Digital Health Equity Initiatives: Legislation allocating funding to expand broadband access and reduce digital health disparities. Since wearables require digital infrastructure and internet connectivity, policies addressing digital divides directly enable broader wearable adoption. Oura has expressed support for these initiatives while emphasizing the importance of including underserved populations in health monitoring implementation.
Public Health Data Governance: Legislation establishing frameworks for how public health agencies can access and use aggregated wearable data for disease surveillance. These policy discussions address when and how de-identified population health data can be shared for public health purposes while maintaining privacy protections.
Healthcare System Transformation Legislation
Broader healthcare reform legislation increasingly addresses digital health and preventive care. While these bills aren't specifically about Oura, the company engages with the legislative process to ensure wearable technology is considered and supported.
Prevention-Focused Healthcare Models: Legislation incentivizing healthcare systems to shift toward prevention. This includes reimbursement reforms, funding for preventive care programs, and regulations encouraging providers to invest in prevention infrastructure. Oura has advocated that continuous monitoring should be considered a key prevention tool.
Healthcare Workforce Development: Legislation supporting training and education for healthcare professionals in digital health. As wearable monitoring becomes more prevalent, providers need training in interpreting wearable data and integrating it into clinical practice. Oura has engaged with healthcare education stakeholders and policymakers about workforce development needs.
Mental Health Parity and Digital Tools: Legislation advancing mental health parity includes provisions about digital health tools for mental health. Oura's research showing relationships between physiological metrics and mental health has been relevant in these discussions.

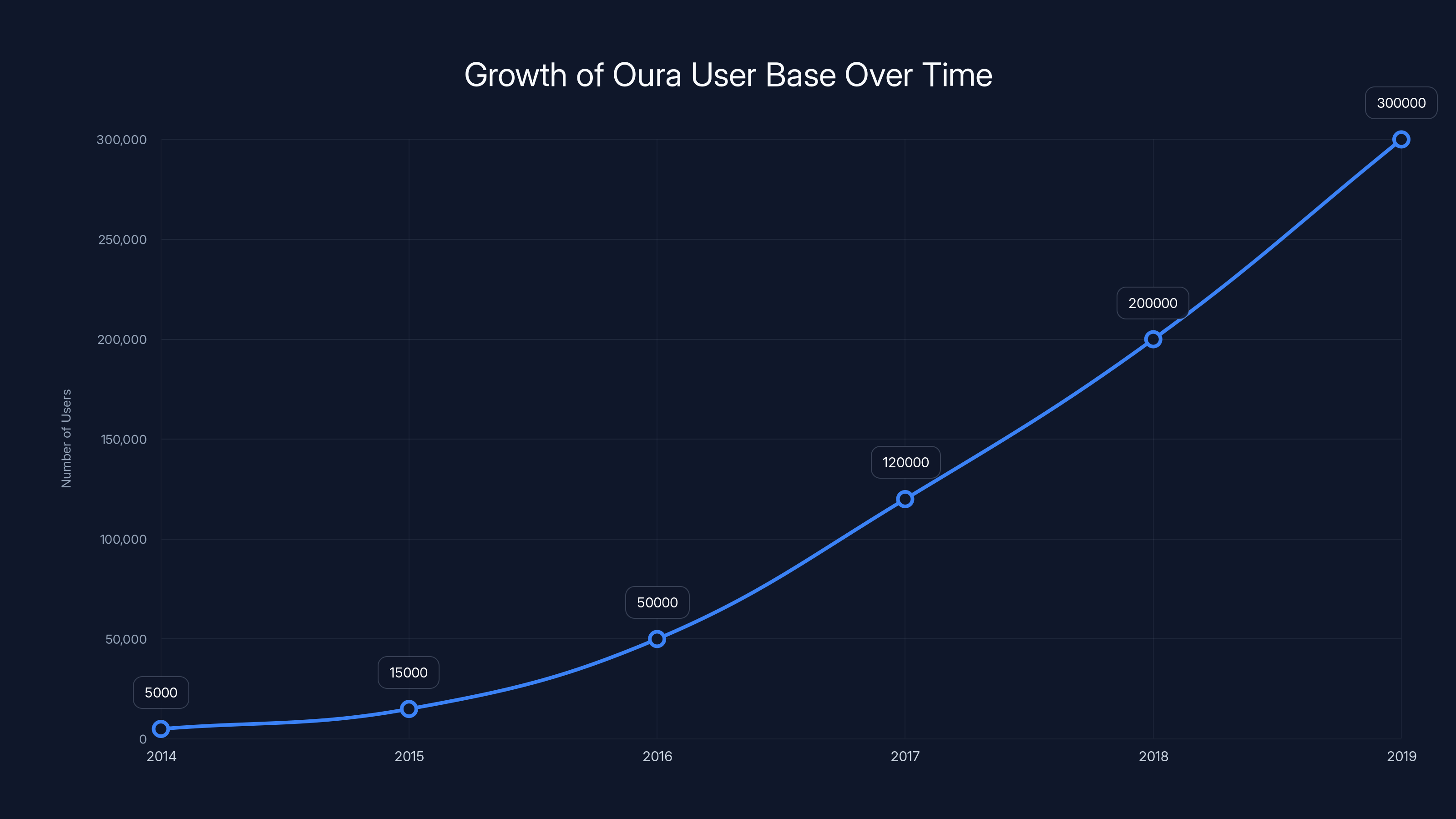
Oura's user base grew significantly from 2014 to 2019, reaching approximately 300,000 users by 2019. This growth reflects the increasing demand for clinically relevant health insights. (Estimated data)
Challenges and Criticisms: Policy Pushback and Ongoing Debates
Privacy and Surveillance Concerns
While Oura's policy engagement has generated significant interest, it also faces substantial criticism and pushback, particularly around privacy and surveillance. These criticisms merit serious consideration as they illuminate real tensions in wearable health monitoring policy.
The fundamental concern is that continuous health monitoring creates surveillance infrastructure that could be misused. Even if Oura itself handles data responsibly, what happens if that data is subpoenaed by law enforcement? What if it's breached and exposed? What if government agencies gain access without proper oversight? History provides cautionary examples: cell phone location data has been extensively accessed by law enforcement with varying degrees of legal justification. Health data could face similar pressures.
Moreover, continuous health data reveals extremely intimate information about individuals' lives. Sleep patterns, stress levels, illness, menstrual cycles, cardiovascular health—all are captured by wearables. This data could be used for discrimination. Insurance companies might access it and adjust premiums. Employers might make decisions about employment based on health metrics. Governments might use it for social control. These aren't hypothetical risks; they're risks that serious policy analysts believe should be taken seriously.
Oura has engaged with these criticisms by emphasizing data governance and proposing strong privacy protections. However, critics argue that no legal framework adequately protects against all surveillance risks. The existence of data creates risk, regardless of current protections. Once collected, data can be accessed through changes in law, breaches, or misuse. Some privacy advocates argue that the default position should be minimizing data collection rather than collecting everything and hoping legal protections prevent misuse.
This creates genuine policy tension: the health benefits of continuous monitoring must be weighed against surveillance and privacy risks. Reasonable people disagree about where the balance should be.
Health Equity and Access Concerns
Another significant line of criticism involves health equity. Critics note that Oura users are predominantly affluent and health-conscious. Early wearable adopters tend to be wealthy, have high health literacy, and live in areas with good digital infrastructure. If wearable-enabled health improvements benefit primarily wealthy populations, this could exacerbate existing health inequities.
Oura has responded by stating commitment to equity and engaging with policymakers on access initiatives. However, critics argue that market-driven approaches to health technology naturally concentrate benefits among the affluent. Achieving equity requires deliberate policy interventions that may not happen without sustained advocacy.
Moreover, even if wearables become available to lower-income populations, benefits might not accrue equally. Health literacy matters—less educated populations might struggle to interpret wearable data and translate it into health behavior change. Digital infrastructure matters—unreliable internet access limits utility. Healthcare access matters—if someone's wearable detects early disease signs but they lack affordable healthcare, the benefit of detection is limited.
These equity concerns are important for policy discussions. Expanding health technology without addressing these underlying factors might create a world where wealthy people benefit greatly while poor people gain little, reinforcing existing health disparities.
Clinical Utility Questions
While Oura can measure physiological parameters with clinical-grade accuracy, questions remain about clinical utility. Can these measurements actually improve health outcomes at population scale? Preliminary research suggests yes, but more evidence is needed.
Some medical professionals are skeptical that continuous monitoring translates to actionable clinical insights for most people. Yes, heart rate variability might decline indicating illness, but most people can already recognize when they're getting sick through symptoms. Does early detection change management? For mild illness, probably not much. For serious illness, probably yes. But which detected illnesses represent serious risk requiring clinical intervention versus self-limited minor illness? This remains unclear for many conditions.
Moreover, continuous monitoring generates information overload. Most health metrics change slightly from day to day due to normal variation, stress, diet, sleep, activity, etc. How do people distinguish meaningful changes from noise? How do clinicians prioritize which changes to act on? These are real challenges that affect clinical utility.
Responsible policy discussions must address these questions. If expanded wearable adoption doesn't actually improve health outcomes, policy investments in enabling this adoption would be misdirected. Policymakers appropriately want evidence that interventions they support actually work before scaling them.

Industry Partnerships and Ecosystem Development
Healthcare System Integration Partnerships
Oura's policy impact extends through partnerships with healthcare systems exploring wearable integration. These partnerships generate real-world evidence about whether continuous monitoring improves health outcomes when integrated into clinical practice. They also demonstrate commitment to healthcare transformation beyond consumer sales.
Several major healthcare systems have launched pilot programs incorporating Oura data into patient care. These programs test questions like: if providers receive alerts about concerning physiological changes, does this enable earlier intervention and better outcomes? If patient data from wearables is integrated into electronic health records, do providers use this information and does it change clinical decisions? How should alerts be designed to be useful rather than overwhelming?
Early results from these pilots appear positive, though larger, more rigorous studies are needed. Healthcare systems report that wearable data provides useful insights about patient status, enables earlier identification of concerning changes, and supports preventive interventions. However, the impacts on hard outcomes like mortality and hospitalization rates remain being studied.
These partnerships matter for policy because they generate evidence of real-world effectiveness. Policymakers care less about clinical studies in research settings than about whether health technology actually improves care in regular healthcare systems. If partnerships show consistent benefits, policy support becomes stronger.
Research Institution Collaborations
Oura has systematically built collaborations with leading research institutions. These collaborations serve multiple functions: they generate evidence supporting Oura's claims, they enable independent researchers to study the technology, and they create credibility in academic communities where policymakers look for guidance.
Notable collaborations include partnerships with major universities and medical centers conducting research on wearable applications in disease detection, prevention, and health behavior change. These research partnerships have produced peer-reviewed publications in prestigious journals. Independent researchers—not Oura employees—examining Oura technology in rigorous studies and publishing results in peer-reviewed venues. This independent validation is important for credibility.
Ecosystem Partnerships
Oura has also engaged with companies and organizations addressing adjacent challenges. For example, partnerships with digital health platforms enable wearable data to connect with apps supporting behavior change, health coaching, and clinical integration. Partnerships with telehealth companies enable remote monitoring to support virtual care. Partnerships with occupational health companies enable workplace wellness applications.
These ecosystem partnerships matter for policy because they demonstrate that wearable technology doesn't exist in isolation. Meaningful health impact requires integration with broader health support infrastructure. Policymakers considering wearable-focused policies must think about this ecosystem dimension.

Global Policy Perspectives: International Approaches to Wearable Health Regulation
European Data Privacy Frameworks
While much policy discussion has focused on the United States, Oura operates globally and engages with policymakers internationally. European approaches to health data regulation differ from the US, providing instructive contrasts.
Europe's General Data Protection Regulation (GDPR) provides stronger consumer data protections than US law. GDPR principles emphasize user control, data minimization, and explicit consent for data use. For health data specifically, GDPR includes special protections recognizing health data's sensitivity. This regulatory framework creates higher privacy standards but potentially greater friction for companies wanting to utilize health data at scale.
Oura has adapted its privacy practices to comply with GDPR while maintaining functionality. The company emphasizes to European policymakers that strong privacy protections and beneficial health technology can coexist. However, European policymakers debate whether current protections are sufficient. Some advocate for even stronger controls, while others worry that excessive regulation stifles innovation.
Oura's engagement in European policy contexts demonstrates how international regulatory variation affects policy strategy. What works politically in the US might not work in Europe. The company must adapt messaging and proposals to local regulatory contexts and political cultures.
Singapore and Nordic Models
Oura has particularly engaged with policymakers in Singapore and Nordic countries (Denmark, Finland, Sweden, Norway). These regions offer interesting case studies for different policy approaches.
Singapore has taken a more techno-friendly regulatory approach, encouraging health technology adoption while implementing strong data governance. The government actively promotes wearable adoption for population health monitoring and has been receptive to companies like Oura partnering with health authorities. This creates policy environment relatively favorable to wearable expansion.
Nordic countries, particularly Finland (Oura's home country), offer models balancing digital innovation with strong privacy protections and social welfare. These countries have explored wearable integration with universal healthcare systems, considering how continuous monitoring might enhance preventive care within public health systems. Oura's engagement with Nordic policymakers involves understanding how their model—publicly-funded healthcare with universal coverage—might incorporate continuous monitoring.
These international policy variations inform global strategy. Oura must navigate different regulatory environments, political cultures, and healthcare systems. Success requires localized understanding and adapted approaches for different policy contexts.

Future Policy Directions: What's Next for Oura and Wearable Health Policy
Emerging Policy Priorities
As Oura's policy engagement matures, several emerging priorities are shaping discussions:
AI and Algorithm Transparency: As AI algorithms become more central to wearable health technology, policy discussions increasingly address algorithmic transparency and accountability. How should algorithms determining health status be validated? What transparency is owed to users about how algorithms work? How should algorithmic bias be addressed? These questions affect not just Oura but the entire sector.
Interoperability Standards: Policy discussions are moving toward requiring standardized data formats enabling wearable data to integrate with diverse healthcare systems, EHRs, and research platforms. This benefits users and researchers while reducing vendor lock-in. Oura has engaged in standards discussions while advocating for standards that maintain security and privacy.
Reimbursement Models: Current healthcare reimbursement inadequately supports preventive care enabled by wearables. Policy discussions address how reimbursement should evolve. Should providers be reimbursed for remote monitoring? Should patients receive coverage for wearables? How should risk-adjustment work in systems where continuous data enables precise individual risk assessment?
Liability and Accountability Frameworks: As wearables become more integrated with healthcare, questions emerge about liability. If wearable data suggests someone should seek care and they don't, who's responsible if they suffer harm? If healthcare providers receive wearable data but don't act on concerning findings, are they liable? Clear liability frameworks would enable broader adoption.
Regulatory Modernization: The FDA regulatory framework predates continuous monitoring devices. Ongoing discussions address how regulation should evolve. Some advocate for lighter-touch regulation for low-risk monitoring while maintaining oversight for clinical recommendations. Others want stronger regulations. These debates will shape what companies like Oura can offer.
Long-Term Vision: Oura's Policy Goals
While specific policy goals shift as circumstances change, Oura's underlying vision for healthcare transformation appears consistent. The company envisions a future where continuous health monitoring becomes standard, enabling healthcare systems to shift from treatment to prevention. In this vision:
- Continuous Monitoring is Universal: Most people wear health monitors, with subsidized access for those unable to afford devices.
- Data Integration: Wearable data integrates seamlessly with healthcare systems, enabling providers to leverage continuous monitoring in clinical practice.
- Prevention is Central: Healthcare systems reorganize around prevention, with continuous data enabling early detection and intervention.
- Equitable Access: Wearable benefits extend across socioeconomic groups, reducing health disparities rather than exacerbating them.
- Privacy is Protected: Strong legal frameworks protect health data from misuse while enabling beneficial research and public health applications.
- Outcomes are Improved: Healthcare costs decrease while health outcomes improve as disease prevention replaces disease treatment.
Achieving this vision requires policy changes at multiple levels: FDA regulatory framework, healthcare reimbursement, data governance, healthcare system structure, and public health infrastructure. Oura's policy engagement aims to influence all these domains.
Whether this vision is achievable remains to be seen. Substantial challenges exist. Policy adoption is slow. Healthcare system change is difficult. Privacy concerns are legitimate. Equity gaps are real. However, Oura's systematic policy engagement suggests the company is committed to the long-term work of shifting healthcare toward prevention.

Emerging Alternatives and Parallel Approaches to Health Monitoring
AI-Powered Health Platforms and Automation Tools
While Oura focuses on hardware-based continuous monitoring, alternative approaches to health transformation are also emerging. Platforms like Runable offer AI-powered automation for health-related tasks, though operating in different domains than physical biometric monitoring. These alternatives represent different strategic approaches to health technology innovation.
AI-powered platforms approach health challenges through content generation, workflow automation, and data analysis rather than physical biometric sensors. For example, such platforms might automate health documentation, generate personalized health reports based on user input, or streamline administrative healthcare workflows. While these don't replace continuous monitoring, they address complementary challenges in healthcare delivery and administration.
For policymakers, understanding this landscape of diverse health technology approaches matters. Rather than betting on single technologies, robust policy frameworks should support multiple approaches addressing different aspects of health challenges. Continuous monitoring addresses physiological early detection. AI automation addresses healthcare delivery efficiency. These can be complementary.
Smartphone-Based Monitoring and Software Solutions
Alternative approaches use smartphones for health monitoring rather than specialized wearables. Smartphones contain sensors enabling health measurement—cameras for measuring heart rate, accelerometers for activity tracking, microphones for respiratory analysis. Software platforms leverage these ubiquitous sensors rather than requiring specialized hardware.
The advantage of smartphone-based approaches is that phones are already widely adopted across all socioeconomic groups. No additional hardware purchase is required. This potentially enables more equitable health monitoring than specialized devices like Oura that require additional investment.
The disadvantage is reduced measurement precision. Specialized sensors in devices like Oura rings achieve higher accuracy than smartphone sensors. For clinical applications requiring high accuracy, smartphones may be insufficient.
Policy discussions increasingly address this hardware-versus-software tradeoff. Should policy favor specialized wearables with high accuracy but limited access? Or less accurate smartphone-based solutions with universal potential access? Reasonable arguments exist on both sides, and policy likely needs to support diverse approaches rather than favoring one.
Clinic-Based and Remote Monitoring Solutions
Another alternative involves clinic-based monitoring where patients visit healthcare facilities for health measurement rather than continuous home monitoring. Remote monitoring through telehealth connects patients with providers between clinic visits, capturing health information through traditional means (patient self-report, vital sign measurement during visits) supplemented by questionnaires or basic home monitoring.
These approaches require less technology infrastructure than wearable-based continuous monitoring but provide less continuous data. They work well for populations with reliable healthcare access but are insufficient for those with limited access.
Policy frameworks should likely support multiple approaches serving different populations and contexts. Universal continuous wearable monitoring might not be optimal for everyone. For some, periodic clinic-based monitoring combined with remote support between visits might be more appropriate and culturally acceptable.

Key Takeaways: What Policymakers Should Understand
The Promise and Peril of Continuous Health Monitoring
Oura's policy engagement illustrates both the significant promise of continuous health monitoring and important legitimate concerns requiring careful policy attention.
The Promise: Continuous biometric monitoring with clinical-grade accuracy enables health paradigm shifts. Early disease detection, prevention-focused healthcare, reduced hospitalizations, improved outcomes, and cost savings all become possible if continuous monitoring is properly integrated into healthcare systems. The evidence supporting these potential benefits is increasingly robust.
The Peril: Continuous monitoring creates surveillance infrastructure with potential for misuse. Privacy concerns are legitimate. Health equity concerns are real. Clinical utility questions remain incompletely answered. Adequate policy frameworks protecting privacy while enabling beneficial use don't yet exist. Healthcare system fragmentation limits wearable data usefulness. These challenges are substantial and shouldn't be minimized.
Policy Principles for Wearable Health Technology
Based on Oura's policy engagement and broader health technology discussions, several policy principles appear important:
Evidence-Based Adoption: Policies should require rigorous evidence that wearable-based interventions improve health outcomes before large-scale adoption. Pilot programs and real-world evidence should inform scaling decisions.
Strong Privacy Protection: Legal frameworks protecting health data should be as strong as or stronger than current protections for other sensitive data. Users should maintain control over health data with explicit consent for use.
Equitable Access: Policies should intentionally address health equity, ensuring wearable benefits extend across socioeconomic groups rather than exacerbating disparities.
Interoperability: Standards should enable wearable data to integrate across healthcare systems and platforms, reducing vendor lock-in while enabling broader health system benefits.
Diverse Approaches: Policies should support multiple approaches to health monitoring rather than favoring single technologies, recognizing that different approaches serve different populations.
Ongoing Evaluation: As wearable technology integrates into healthcare, ongoing evaluation of impacts on health outcomes, costs, disparities, and privacy should inform policy refinement.

Conclusion: The Intersection of Innovation and Policy
Oura's systematic policy engagement represents a case study in how health technology companies can influence healthcare policy through evidence, relationships, and strategic communication. The company hasn't achieved all its policy goals, nor has it done so without criticism. However, Oura has succeeded in establishing continuous health monitoring as a legitimate topic in healthcare policy conversations at federal and state levels.
This engagement matters because the future of healthcare increasingly depends on how health technology integrates into health systems. Policymakers making decisions about healthcare regulation, reimbursement, data governance, and system transformation need technical expertise and evidence about what technology can accomplish. Companies like Oura, through systematic policy engagement, provide this information.
However, responsible policy also requires critical questioning. Not all of Oura's proposed policies serve all stakeholder interests equally. Privacy advocates rightfully raise concerns about surveillance risks. Equity advocates appropriately question whether market-driven wearable adoption will reduce health disparities. Healthcare economists validly ask whether benefits justify investments. Clinicians reasonably want evidence that continuous monitoring actually improves care.
The path forward likely involves balanced approaches. Continuous health monitoring has genuine potential to improve healthcare. But realizing this potential requires thoughtful policy addressing privacy, equity, interoperability, and clinical utility. It requires supporting Oura and similar companies while maintaining skeptical scrutiny of their claims and proposals.
For those following healthcare policy, understanding Oura's engagement provides insight into how health technology will likely evolve and how policy decisions now shape healthcare systems for decades to come. The questions policymakers are debating—how to enable innovation while protecting privacy, how to ensure equitable access, how to measure real-world effectiveness, how to govern data responsibly—are fundamentally important questions that will define healthcare's future.
Oura's long-term vision of shifting healthcare toward prevention through continuous monitoring is compelling. Whether this vision becomes reality depends on evidence, policy, implementation, and equity. The coming years will reveal whether continuous health monitoring lives up to its promise or faces fundamental limitations preventing broader adoption. Policy decisions made now will significantly influence this trajectory, making Oura's policy engagement and the broader policy discussions it's catalyzing genuinely consequential for the future of American healthcare.
FAQ
What is a smart health ring and how does it measure biometric data?
A smart health ring is a wearable device worn on the finger that continuously measures physiological metrics including heart rate, heart rate variability, skin temperature, sleep stages, and respiratory rate. The ring contains specialized sensors positioned close to blood vessels in the finger, enabling precise biometric measurement. Algorithms process the sensor data to extract meaningful health insights, such as detecting early illness signs or analyzing sleep quality. Unlike smartwatches that measure similar metrics, rings provide superior measurement accuracy due to their positioning closer to major arteries.
How is Oura influencing healthcare policy and legislation?
Oura influences healthcare policy through multiple channels: providing technical expertise and evidence to policymakers, partnering with research institutions to generate peer-reviewed studies, engaging with legislators on regulatory frameworks for wearable devices, contributing to discussions about healthcare system transformation toward prevention, and collaborating with healthcare systems on real-world implementation. The company provides data and evidence demonstrating that continuous health monitoring can detect illness early, potentially reduce healthcare costs, and support preventive care. These evidence-based conversations with policymakers shape developing legislation around wearable regulation, health data governance, and digital health infrastructure.
What evidence supports using wearables for disease detection?
Multiple peer-reviewed studies demonstrate wearable effectiveness for disease detection. Research shows that heart rate variability, sleep metrics, and skin temperature changes detected by devices like Oura can identify respiratory infections and COVID-19 an average of 1.5 days before symptom onset with detection sensitivity and specificity exceeding 85-90%. Studies validate that physiological changes captured by wearables correlate with health outcomes including cardiovascular function, immune response, and stress levels. Real-world data from large user populations shows that wearable-engaged users experience measurable improvements in sleep, stress, and self-reported health. While more research on long-term health outcomes is ongoing, accumulated evidence supports wearable technology's capability for early detection and health improvement.
What are the primary privacy concerns regarding continuous health monitoring?
Key privacy concerns involve data collection scope (continuous monitoring creates extensive intimate health data), data security vulnerability (breaches could expose sensitive health information), unauthorized access risks (law enforcement or insurance companies might inappropriately access data), and surveillance potential (continuous monitoring creates infrastructure potentially enabling state or corporate health surveillance). Additionally, concerns exist about data permanence—once collected, health data might be accessed through future legal changes, company misuse, or data sales despite current protections. While Oura implements strong privacy practices, critics argue that data collection risk cannot be entirely eliminated through governance frameworks alone, making some level of surveillance risk inherent to continuous monitoring systems.
How could wearable health monitoring reduce healthcare costs?
Wearable monitoring potentially reduces costs through multiple mechanisms: early disease detection enables less intensive interventions (outpatient treatment rather than hospitalization, preventive care rather than acute emergency care), illness prevention through behavior change supported by health data, reduced unnecessary healthcare utilization (addressing health concerns before they become emergencies), and optimized healthcare resource allocation based on population health data. For example, preventing Type 2 diabetes progression through early detection and intervention costs
What regulatory barriers exist for wearable health technology?
The FDA regulatory framework predates continuous monitoring devices, creating uncertainty about classification and approval pathways. Current regulations were designed for static diagnostic devices rather than dynamic systems with continuously updating algorithms. Regulatory questions include whether continuous monitoring devices should require FDA approval and at what classification level, how algorithmic updates should be regulated, what evidence standards should apply, and how clinical claims should be validated. Existing regulatory pathways impose substantial costs and delays that might stifle innovation in wearables. Policymakers are discussing regulatory modernization creating pathways specifically for continuous monitoring devices while maintaining safety and efficacy oversight. Clarity on regulatory requirements would accelerate healthcare system integration of wearables.
How might wearable technology contribute to health equity improvements or worsen disparities?
Wearables could improve equity by enabling early detection in underserved populations with limited healthcare access, identifying health conditions that would otherwise go undiagnosed, and supporting preventive care for populations currently receiving primarily acute care. However, without intentional policy efforts, wearables might worsen equity given current adoption concentrates among affluent, health-literate populations with good digital infrastructure. Health literacy differences, digital infrastructure disparities, and limited healthcare access in underserved communities could prevent disadvantaged groups from translating wearable data into health improvements. Responsible policy requires subsidized access programs, inclusive research ensuring wearable effectiveness across demographic groups, and healthcare system integration enabling wearables to support care for underserved populations.
What is the difference between continuous monitoring and traditional healthcare assessment?
Traditional healthcare involves episodic encounters: annual checkups, clinic visits when symptoms appear, or emergency department visits for acute problems. Assessment occurs at specific points in time with months or years between evaluations. By contrast, continuous monitoring generates health data every minute across months and years. This enables detecting gradual physiological changes that episodic assessment misses, identifying disease early before symptoms appear, tracking response to interventions in real-time, and recognizing patterns in health that appear only with extended observation. Continuous monitoring enables proactive, prevention-focused care versus reactive, treatment-focused care. However, continuous monitoring generates information overload requiring algorithmic support to identify meaningful changes. Both approaches have roles; optimal healthcare might integrate both episodic clinical assessment and continuous monitoring data.
What role might wearables play in workplace health and productivity?
Wearables could support workplace health by identifying employees developing illness (enabling early intervention before serious disease), monitoring stress and sleep patterns (identifying burnout and enabling support), tracking activity and promoting movement breaks (addressing sedentary behavior), and providing occupational health data supporting workplace safety improvements. Aggregate, de-identified wearable data could reveal workplace health trends (ergonomic problems, stress factors, health risks) enabling targeted improvements. The case is economically compelling: improving sleep, reducing stress, and preventing illness generates measurable productivity improvements and reduced healthcare costs. Some employers have begun offering wearables as wellness benefits. However, employee privacy concerns exist regarding employer access to personal health data, requiring careful governance ensuring benefits without inappropriate health-related employment decisions.
How do Runable and other AI automation platforms complement wearable health technology?
While wearables like Oura focus on continuous biometric measurement and early detection, AI automation platforms address complementary healthcare challenges. Platforms like Runable offer AI-powered document generation, workflow automation, and health-related task automation that streamline healthcare delivery and administration. These tools might automate health report generation, clinical documentation, patient communication, or health data analysis—tasks that consume healthcare professional time but don't require clinical judgment. Combining continuous biometric monitoring (Oura) with AI-powered health automation (Runable) creates comprehensive health system improvements: early detection combined with efficient care delivery. Policymakers increasingly recognize that health system transformation requires both better information (continuous monitoring) and more efficient processes (AI automation), supporting diverse technological approaches serving different healthcare functions.

Summary: The Path Forward
Oura's policy engagement demonstrates how wearable health technology can influence healthcare policy through evidence, expertise, and strategic relationships. The company has positioned continuous health monitoring as a legitimate policy topic while maintaining focus on research evidence and clinical utility. However, significant policy questions remain: How should privacy be protected while enabling beneficial health monitoring? How can health equity be ensured? What regulatory frameworks should govern wearables? How should healthcare systems integrate continuous monitoring data? How should reimbursement evolve to support prevention?
These questions don't have simple answers, but Oura's engagement contributes sophisticated perspectives to policy discussions. As healthcare increasingly leverages health technology, policymakers will continue navigating tensions between innovation and protection, efficiency and equity, individual choice and population health. Understanding how companies like Oura approach policy—through evidence, relationships, and balanced advocacy—provides insight into how health technology's future will be shaped.
The emerging healthcare landscape will likely involve multiple health monitoring approaches, diverse automation tools, and complex policy frameworks balancing innovation with protection. Oura's vision of prevention-focused healthcare enabled by continuous monitoring may partially materialize, modified through policy processes to address equity, privacy, and clinical utility concerns. The coming years will reveal whether continuous health monitoring's promise justifies the policy attention and resources being directed toward it.

Related Articles
- Garmin Cirqa Smart Band: Complete Analysis & Alternatives [2025]
- How to Track Sleep in Apple Health: Complete Guide [2025]
- Tech News January 2025: Samsung S26 & Garmin Whoop Features
- Apple's AI Pin Strategy: Why It Misses the Mark [2025]
- Mentra Live Smart Glasses: Open-Source AR & App Store Guide [2025]
- Amazon Bee AI Wearable: Complete Guide & Alternatives [2025]




