Measles Resurgence: A Grim Warning for Future Pandemics [2025]
In 2000, the United States declared measles eliminated, a significant public health achievement. However, recent outbreaks have reignited concerns about infectious disease control, signaling vulnerabilities that could affect the global health landscape. This article delves into the reasons behind the resurgence of measles, its implications for future pandemics, and the strategies necessary to prevent further outbreaks.
TL; DR
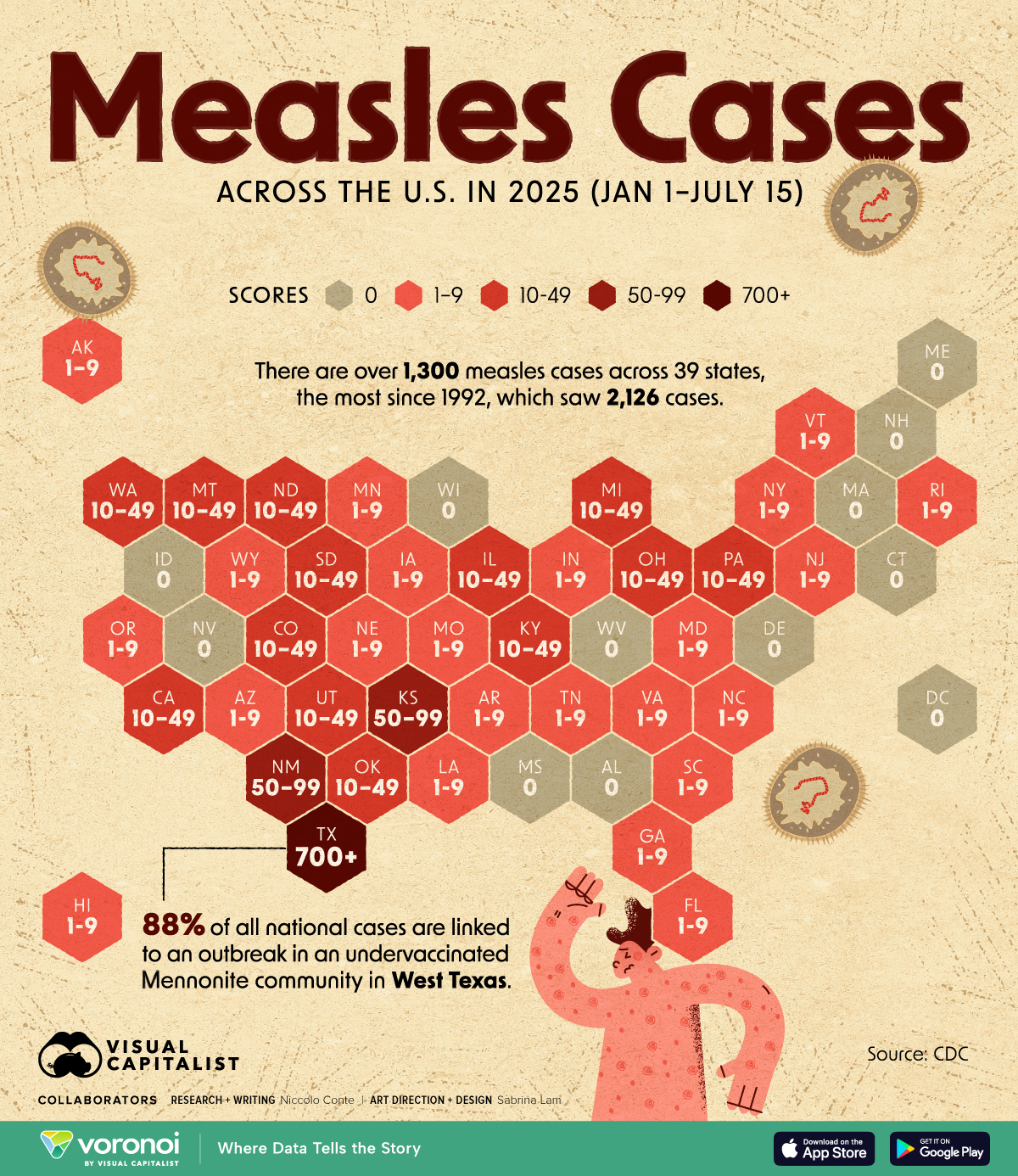
- Measles Outbreaks: Over 1,300 cases reported in the US in 2026, with persistent circulation across multiple states, as noted by the Center for Infectious Disease Research and Policy.
- Vaccination Gaps: Declines in vaccination rates due to misinformation and access issues are primary causes, according to the Infectious Diseases Society of America.
- Public Health Systems: Current systems are struggling to manage infectious disease surveillance and response.
- Global Implications: Measles resurgence highlights global vulnerabilities in pandemic preparedness.
- Actionable Solutions: Strengthening vaccination programs and improving public health infrastructure is critical.
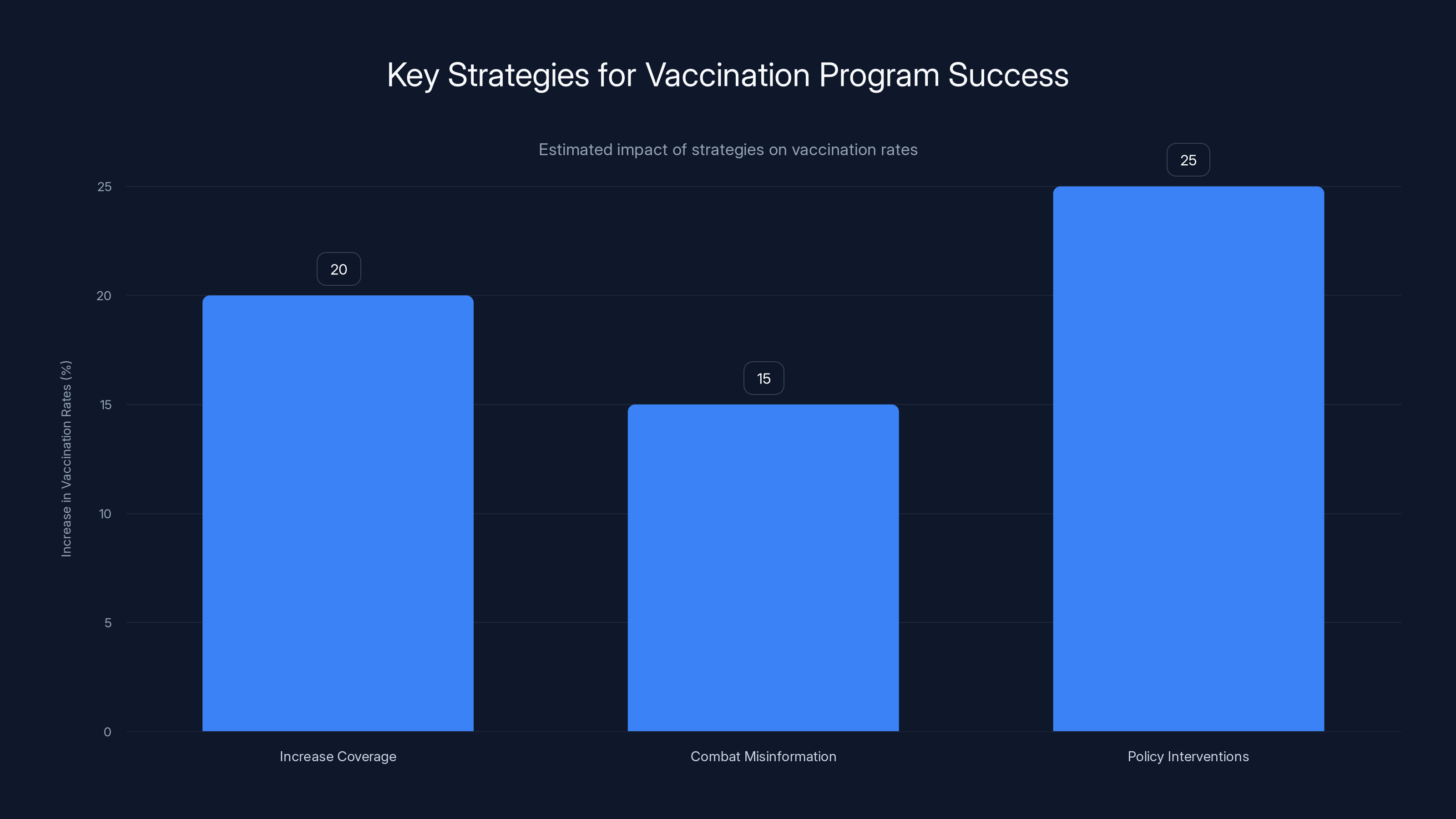
Implementing policy interventions is estimated to have the highest impact on increasing vaccination rates, followed by increasing coverage and combating misinformation. Estimated data.
Understanding Measles and Its Historical Context
Measles is a highly contagious viral disease characterized by fever, cough, and a characteristic rash. It can lead to severe complications, including pneumonia, encephalitis, and death. Historically, measles has been a significant cause of childhood mortality worldwide, but the development of the measles vaccine in 1963 dramatically reduced its incidence.
The Path to Elimination
The US achieved measles elimination in 2000, meaning the disease was no longer endemic. This success was largely due to widespread vaccination campaigns and robust public health infrastructure. However, the term "elimination" does not mean eradication; measles can still be imported from other countries.
Recent Resurgence
The resurgence of measles in the US is alarming. From 1993 to 2024, the country reported a few hundred cases annually. However, as of 2026, measles has been continuously circulating for over a year, affecting 47 states since 2025. Significant outbreaks have occurred in Texas, Utah, Arizona, and South Carolina, as reported by Florida Phoenix.
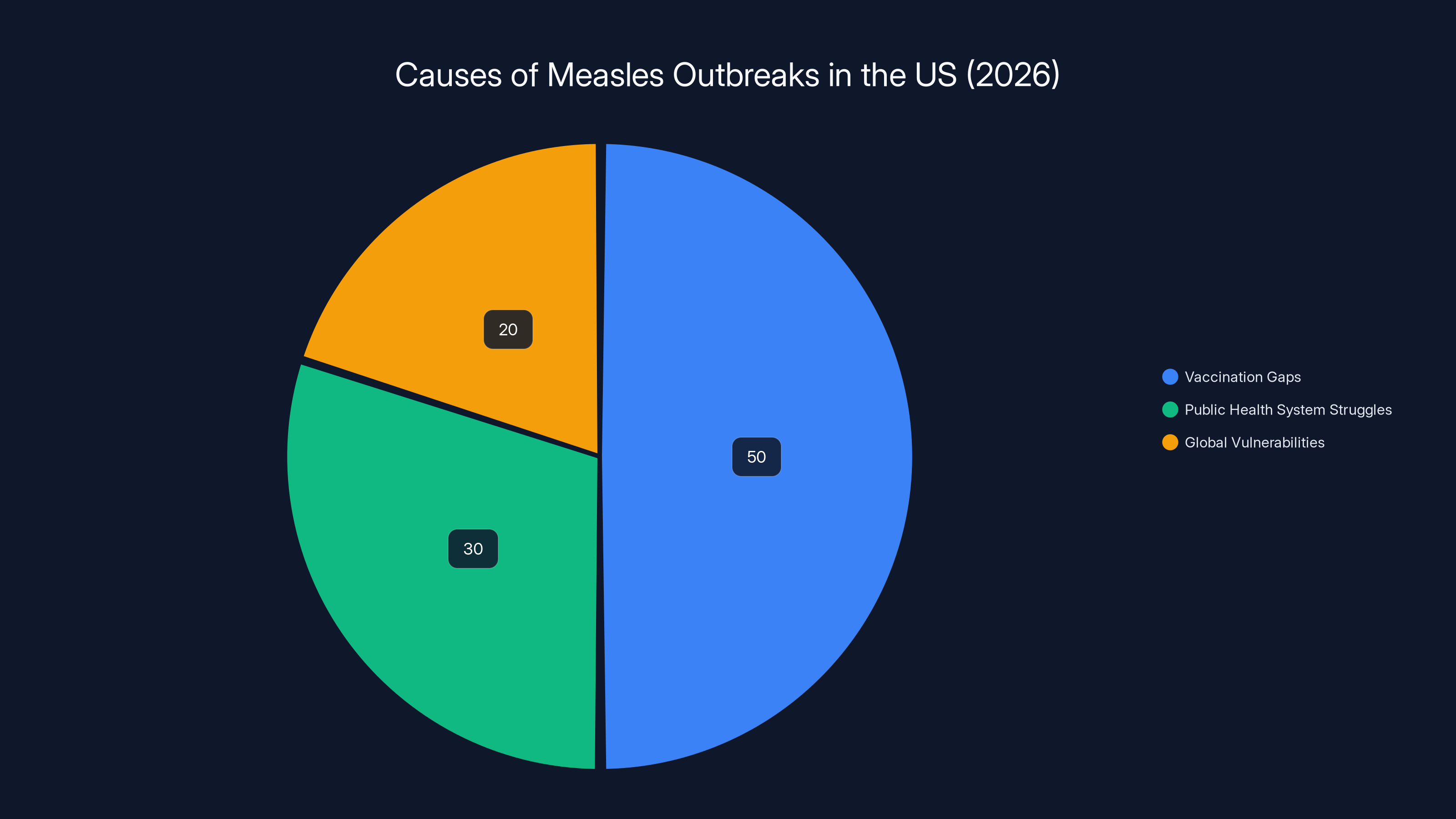
Estimated data shows vaccination gaps are the leading cause of measles outbreaks, followed by public health system struggles and global vulnerabilities.
Causes of the Measles Resurgence
Decline in Vaccination Rates
One of the primary factors in the resurgence of measles is the decline in vaccination rates. Vaccine hesitancy, fueled by misinformation and distrust in medical institutions, has led to decreased immunization coverage.
- Misinformation: The spread of false information about vaccine safety has led to public skepticism, as highlighted by MedRxiv.
- Access Issues: Socioeconomic and logistical barriers prevent some populations from accessing vaccines, according to Infectious Disease Advisor.
Gaps in Public Health Infrastructure
The resurgence also highlights gaps in public health infrastructure. Many areas lack the resources to effectively monitor, respond to, and prevent outbreaks.
- Surveillance Limitations: Inadequate disease surveillance systems hinder timely outbreak detection and response, as noted by CIDRAP.
- Funding Cuts: Reduced funding for public health initiatives has weakened the capacity to maintain high vaccination rates.
Global Travel and Importation
Global travel facilitates the importation of measles cases. Travelers from countries with ongoing measles transmission can introduce the virus into communities with low vaccination coverage, as reported by the CDC.

Implications for Future Pandemics
Increased Vulnerability
The resurgence of measles is a stark reminder of our vulnerability to infectious diseases. It underscores the need for robust public health systems capable of managing emerging threats, as emphasized by UCHealth.
Lessons for Pandemic Preparedness
The current measles situation offers critical lessons for pandemic preparedness:
- Strengthening Surveillance: Investing in advanced surveillance technologies can improve outbreak detection and response.
- Enhancing Communication: Clear and transparent communication strategies are essential to combat misinformation, as discussed by WesternU News.
01840-2/asset/59d4ce1d-0ca6-411f-90ab-8c639198e673/main.assets/gr1_lrg.jpg)
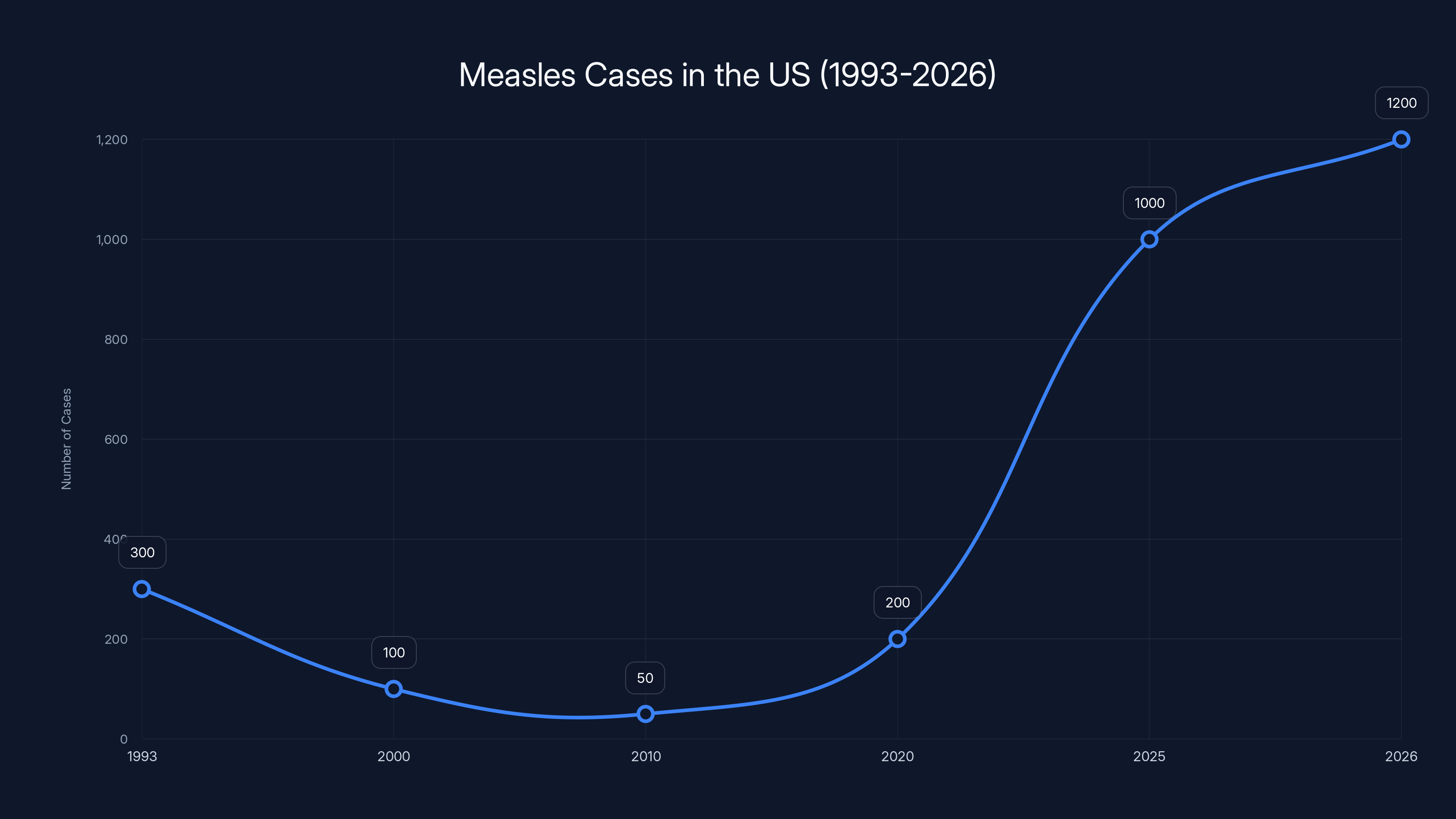
The chart shows a significant increase in measles cases in the US from 2020 to 2026, highlighting a resurgence after years of low incidence. Estimated data.
Practical Strategies for Prevention and Control
Strengthening Vaccination Programs
To prevent future outbreaks, it is essential to strengthen vaccination programs:
- Increase Coverage: Implement targeted campaigns to increase vaccination rates, especially in underserved communities.
- Combat Misinformation: Utilize digital platforms to disseminate accurate information about vaccine safety and efficacy.
- Policy Interventions: Introduce policies that encourage or mandate vaccination for school entry.
Enhancing Public Health Infrastructure
Robust infrastructure is crucial for managing disease outbreaks:
- Invest in Technology: Deploy AI and data analytics for real-time disease tracking and prediction.
- Resource Allocation: Ensure adequate funding for public health departments to maintain essential services.

Future Trends and Recommendations
Emerging Technologies in Disease Control
Advancements in technology offer new possibilities for disease control:
- AI in Epidemiology: AI can identify patterns in disease spread, enabling proactive measures.
- Genomic Surveillance: Genome sequencing can track virus mutations and inform vaccine updates.
Global Collaboration
Addressing global health challenges requires collaboration:
- International Partnerships: Countries must work together to share data and resources.
- Global Vaccination Initiatives: Support global efforts to increase vaccine access in low-income regions, as highlighted by the CDC.
Conclusion: Building a Resilient Future
The resurgence of measles is a grim reminder of the constant threat posed by infectious diseases. However, it also presents an opportunity to strengthen our public health systems and improve global health security. By investing in vaccination programs, enhancing public health infrastructure, and leveraging technology, we can build a more resilient future capable of withstanding future pandemics.

FAQ
What is measles?
Measles is a highly contagious viral disease characterized by fever, cough, and a distinctive rash. It can lead to severe complications, including pneumonia and encephalitis.
How does measles spread?
Measles spreads through respiratory droplets when an infected person coughs or sneezes. It can also linger in the air for up to two hours after an infected person has left the area.
Why has measles re-emerged in the US?
The resurgence is largely due to declining vaccination rates, fueled by misinformation and access issues, as well as gaps in public health infrastructure.
How can we prevent future measles outbreaks?
Preventing future outbreaks requires strengthening vaccination programs, combating misinformation, and enhancing public health infrastructure.
What role does global travel play in measles transmission?
Global travel facilitates the importation of measles cases from countries with ongoing transmission, introducing the virus into communities with low vaccination coverage.
How can technology aid in disease control?
Technology, such as AI and genomic surveillance, can aid in disease tracking, prediction, and response, enabling more effective control measures.
Key Takeaways
- Over 1,300 measles cases reported in the US by 2026.
- Vaccine hesitancy and access issues drive resurgence.
- Public health systems face challenges in outbreak management.
- Global travel increases risk of disease importation.
- Strengthening vaccination programs is critical for prevention.
- Technology can enhance disease surveillance and response.
Related Articles
- AI in Epidemiology: How ChatGPT Could Transform Outbreak Investigations [2025]
- CDC Leadership Crisis: The Ongoing Instability Threatening Public Health [2025]
- How Technology Is Revolutionizing Sleep Apnea Treatment [2025]
- Amazon Expands Healthcare AI Assistant Across Its Platform [2025]
- Revolutionizing Women's Health: Whoop's New Blood Test Initiative [2025]
- Explainable AI is Making Black Box Models Obsolete in the Agentic Era [2025]
![Measles Resurgence: A Grim Warning for Future Pandemics [2025]](https://tryrunable.com/blog/measles-resurgence-a-grim-warning-for-future-pandemics-2025/image-1-1773328174066.jpg)



