At-Home STI Tests: Complete Guide to Pros, Cons & Best Options [2026]
Testing for sexually transmitted infections doesn't have to be uncomfortable, time-consuming, or public. For years, people avoided STI testing because of stigma, inconvenience, or sheer anxiety about sitting in a doctor's office while explaining their sexual history to a stranger.
But that's changed. The at-home STI testing market has exploded over the past five years, with dozens of options now available online, at pharmacies, and even through Amazon. These tests use the same laboratory technology as clinic-based testing, which means you get accuracy without leaving your bedroom.
Here's the reality: at-home STI testing works. Really works. But it's not a perfect solution for everyone, and understanding the limitations is just as important as understanding the benefits. Some tests take 30 minutes. Others take five business days. Some cost under
This guide breaks down everything you need to know about at-home STI testing in 2026: what tests actually work, when you should use them, what the data shows about accuracy, and most importantly, when you should absolutely skip the at-home option and see a medical professional instead.
TL; DR
- At-home STI tests are increasingly accurate when you use FDA-approved kits from reputable companies, matching lab-based testing accuracy for bacterial infections like chlamydia, gonorrhea, and syphilis
- Bacterial infections are easier to detect at home than viral infections, making tests for herpes, HIV, and hepatitis less reliable without professional administration
- Turnaround times vary drastically, from 30 minutes (rapid PCR tests) to 5+ business days (mail-in tests), affecting when you'll know your status
- Costs range from 400, but many tests qualify as FSA/HSA-eligible, and insurance may cover them depending on your plan and risk factors
- A positive result still requires professional follow-up, meaning you'll contact a doctor or telehealth provider anyway for treatment, making cost-benefit analysis important
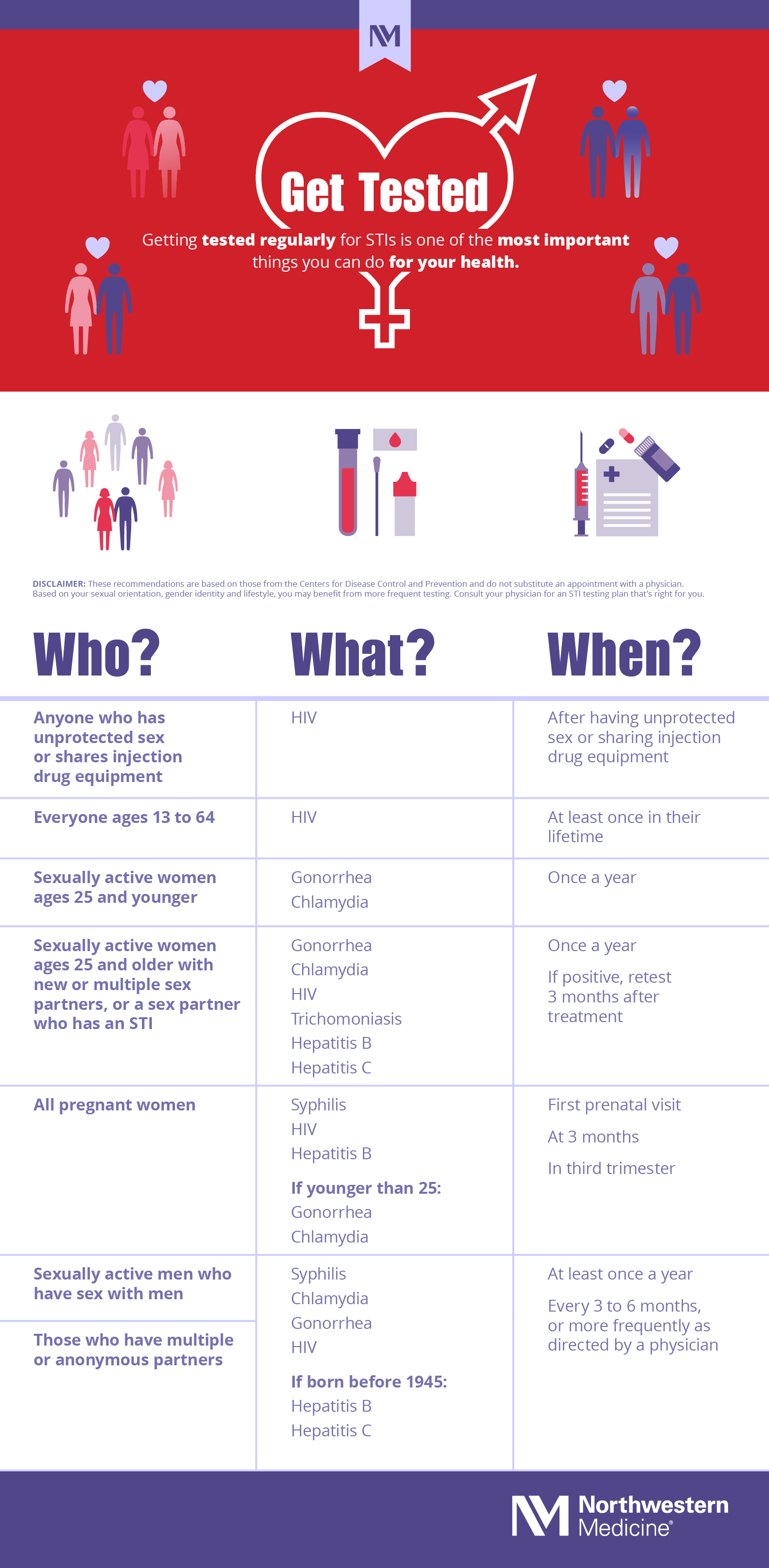

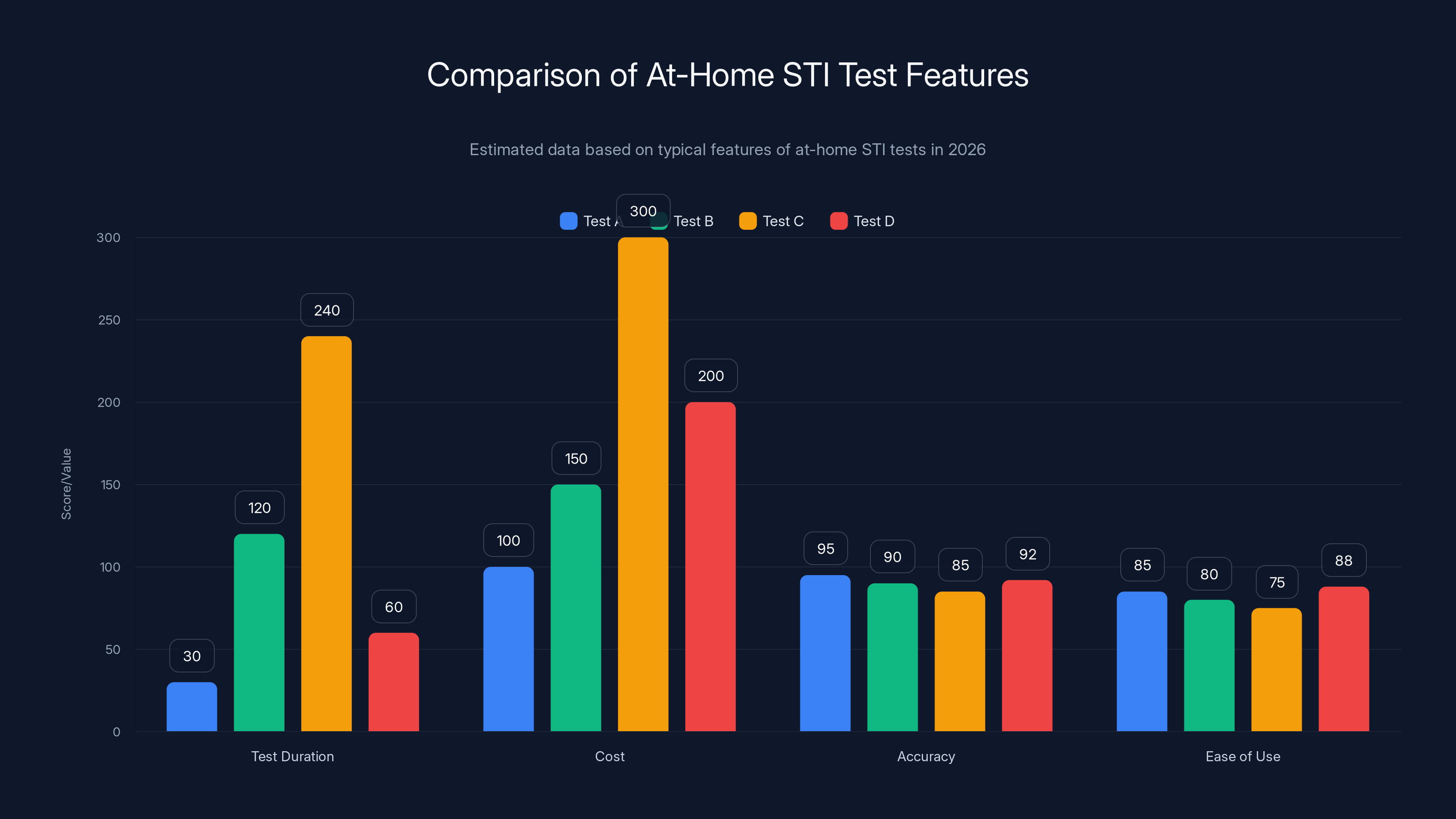
Estimated data shows a range of features for at-home STI tests, with varying durations, costs, and accuracy. Test A offers the quickest results at a lower cost, while Test C is the most expensive and time-consuming.
What Exactly Are At-Home STI Tests?
At-home STI tests are self-administered diagnostic kits that detect sexually transmitted infections using samples you collect yourself. Unlike previous generations of home health tests that were crude approximations, modern at-home STI tests use the exact same laboratory technology—nucleic acid amplification testing (NAAT), enzyme immunoassays, and rapid PCR—that clinics and hospitals use.
The fundamental difference is collection location and timing, not the underlying science. You're doing the sample collection that a nurse or doctor would normally handle. That single difference is why accuracy depends almost entirely on following instructions properly.
How the Collection Process Works
Sample collection varies by test type. For bacterial infections like chlamydia and gonorrhea, you'll typically collect urine in a cup or use a swab to collect samples from the urethra, vagina, rectum, or throat. Some tests offer single-site collection (just urine, for example), while others provide "three-site" kits that let you test multiple locations simultaneously.
You'll use provided materials: sterile swabs that feel like Q-tips, finger-prick lancets for blood samples, or collection cups. The kit includes detailed instructions with photos or videos. Once you've collected samples, you either place them in a provided device that processes results at home, or seal them in a pre-paid mailer envelope and send them to a certified laboratory.
Results arrive in your smartphone app, email, or online portal. If you test positive, most services connect you with a telehealth provider who can prescribe treatment, discuss next steps, and potentially counsel partners about potential exposure.
Why These Tests Work (Or Don't)
The science behind at-home STI testing is straightforward. Sexually transmitted infections leave detectable biological markers in your body: bacterial DNA for chlamydia and gonorrhea, antibodies for HIV, viral particles for herpes. Home test manufacturers don't invent new detection methods; they adapt existing laboratory techniques into consumer-friendly formats.
Accuracy hinges on three factors: the underlying test methodology (which is solid), proper sample collection (which is where failures happen), and testing for infections at appropriate times after exposure. Bacterial infections become detectable within two to three weeks of infection. Viral infections have longer window periods, sometimes up to three months for HIV, which is why home HIV tests are less ideal than professional testing with proper counseling about window periods.

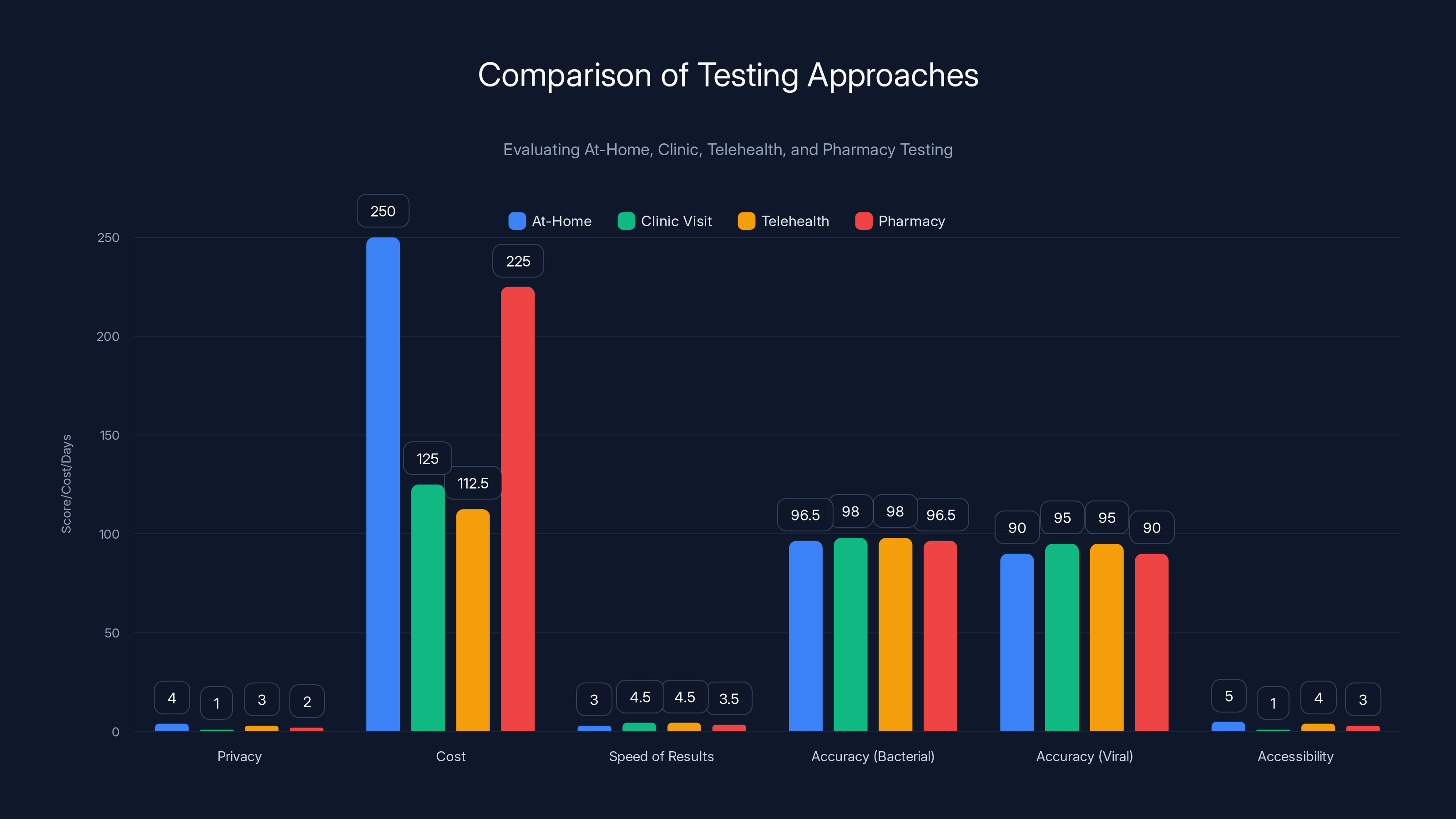
This chart compares testing methods across key factors like privacy, cost, speed, and accuracy. At-home tests excel in privacy and accessibility, while clinics offer the highest accuracy. Estimated data for cost and speed.
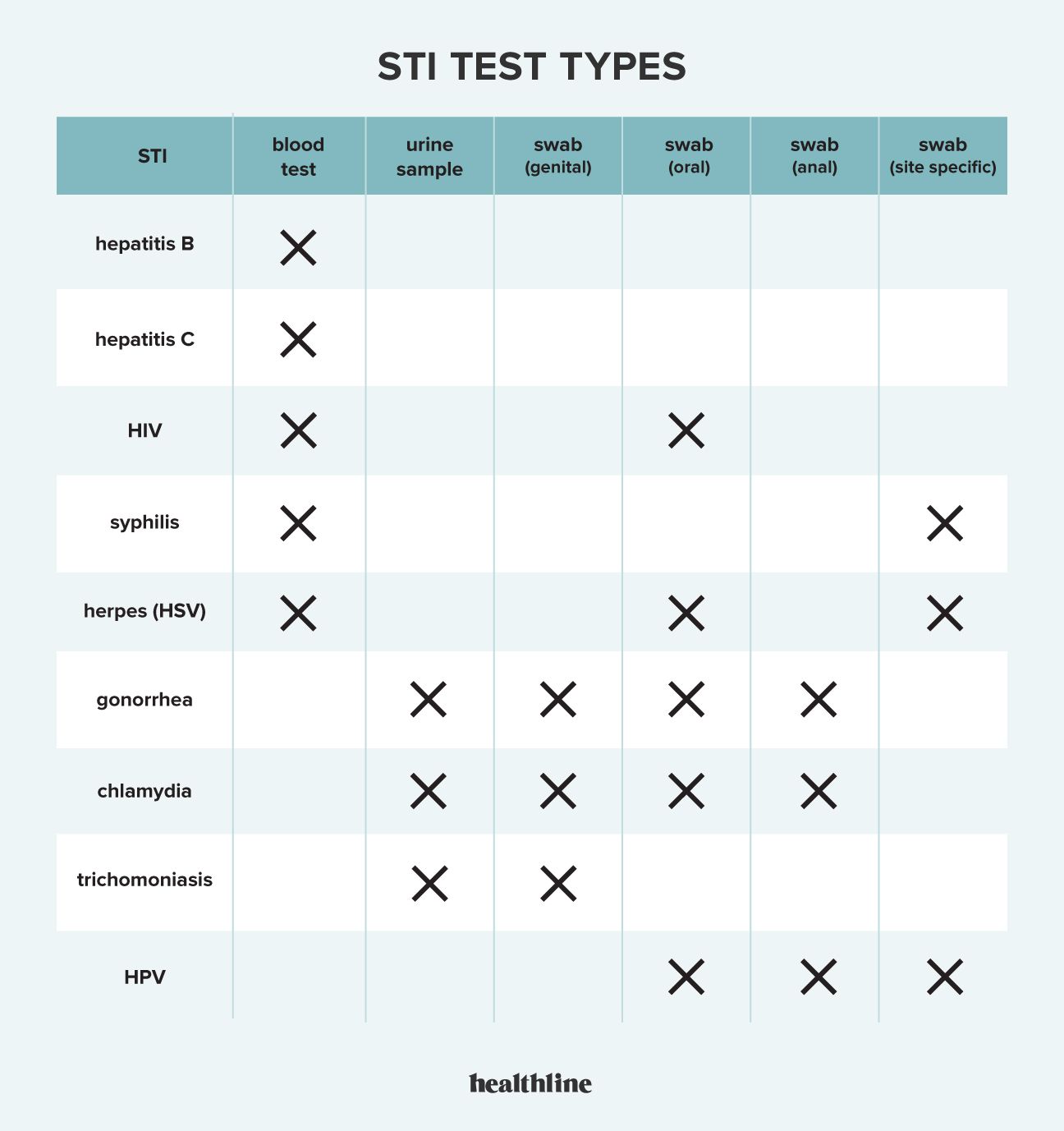
What Infections Can You Actually Test For at Home?
Not all STIs are created equal when it comes to at-home testing. Bacterial infections are far more reliably detected. Viral infections are trickier.
Bacterial Infections (Most Reliable)
Chlamydia and Gonorrhea are by far the most commonly tested STIs at home, and for good reason. Both are bacterial, easily detected via urine or swab samples, and represent the two most frequently diagnosed STIs in the United States. Most at-home test kits screen for both simultaneously. They're accurate in 95-98% of cases when samples are collected properly.
Syphilis testing at home is possible but less common. Most at-home tests use a rapid plasma reagin (RPR) or treponemal test that detects antibodies to the syphilis bacteria. These tests work, but syphilis requires careful interpretation because positive results need confirmation with additional testing, and syphilis progression affects treatment urgency. Many medical professionals prefer seeing patients in person for syphilis diagnosis because it requires discussion of infection history and stage.
Trichomoniasis can be detected at home through wet mount microscopy or nucleic acid testing, depending on the kit. It's less commonly offered than chlamydia/gonorrhea testing, but some comprehensive kits include it.
Viral Infections (Less Reliable at Home)
HIV testing is available in at-home formats, but understanding limitations is critical. Home HIV tests detect antibodies (the immune system's response to HIV infection) 18-45 days after exposure, depending on individual immune response. This "window period" is why professionals recommend testing at 3, 6, and 12 weeks after potential exposure. At-home tests can't counsel you about this window period the way a clinic visit would, potentially leading to false reassurance. Additionally, if you test positive at home, you absolutely must follow up with a professional for confirmation testing and discussion of treatment options.
Herpes home tests are available but less sensitive than professional testing. Herpes is trickier because it hides in nerve cells and may not be detectable during asymptomatic periods. Many infectious disease specialists don't recommend routine home screening for herpes unless you have specific symptoms.
Hepatitis C can be detected at home through antibody testing, and this is actually one area where home testing makes sense because hepatitis C progresses silently. If you think you might have been exposed (sharing needles, blood contact), at-home testing could catch something a doctor might miss if you avoid medical care out of fear.

The Major Advantages of At-Home STI Testing
Convenience is the obvious benefit, but the real advantages run deeper. At-home STI testing removes multiple barriers that prevent people from testing in the first place.
Privacy and Discretion
STI stigma remains real in 2026, regardless of public health messaging that testing is responsible and normal. At-home tests arrive in unmarked or discreet packaging. You collect samples in your own bathroom at midnight if you want. No one at work or home needs to know you're testing (unless you want them to). This privacy is genuinely life-changing for people in conservative communities, those with abusive partners who monitor their healthcare, or individuals who feel ashamed despite knowing rationally that STIs are medical conditions, not moral failings.
The discretion extends to results. You check your phone app rather than calling a clinic nurse who might leave voicemails or send letters that others could see.
Time and Accessibility
Making a doctor's appointment often means waiting weeks. You need to take time off work. You need transportation. You might need childcare. At-home tests eliminate these barriers entirely. You order online, samples arrive in 1-2 days, you test at your convenience, and results come back without a single appointment.
For people in rural areas, those without reliable transportation, shift workers, or anyone with limited healthcare access, at-home testing is genuinely more accessible than traditional testing.
Speed of Results
Some at-home tests provide results in 30 minutes. The rapid PCR options work similarly to at-home COVID tests: you collect a sample, place it in a device, and get results quickly. This matters if you're recently single, entering a new relationship, or practicing responsible hookup culture and want to know your status before sexual activity.
Mail-in tests take 3-5 business days, which is slower than clinic testing but still reasonable and faster than getting an appointment in many areas.
Cost Considerations
At-home STI tests cost
If you're uninsured or underinsured, at-home testing might actually be more affordable than traditional clinic testing, especially if it's a cash visit at an urgent care or clinic.
Comfort and Control
Many people experience real anxiety in medical settings. Anxiety is legitimate and common. At-home testing eliminates white-coat syndrome, the discomfort of discussing sexual history with a stranger, and the vulnerability of examination. You control the pace, the timing, and the environment. This psychological comfort alone makes testing more likely for anxious people.
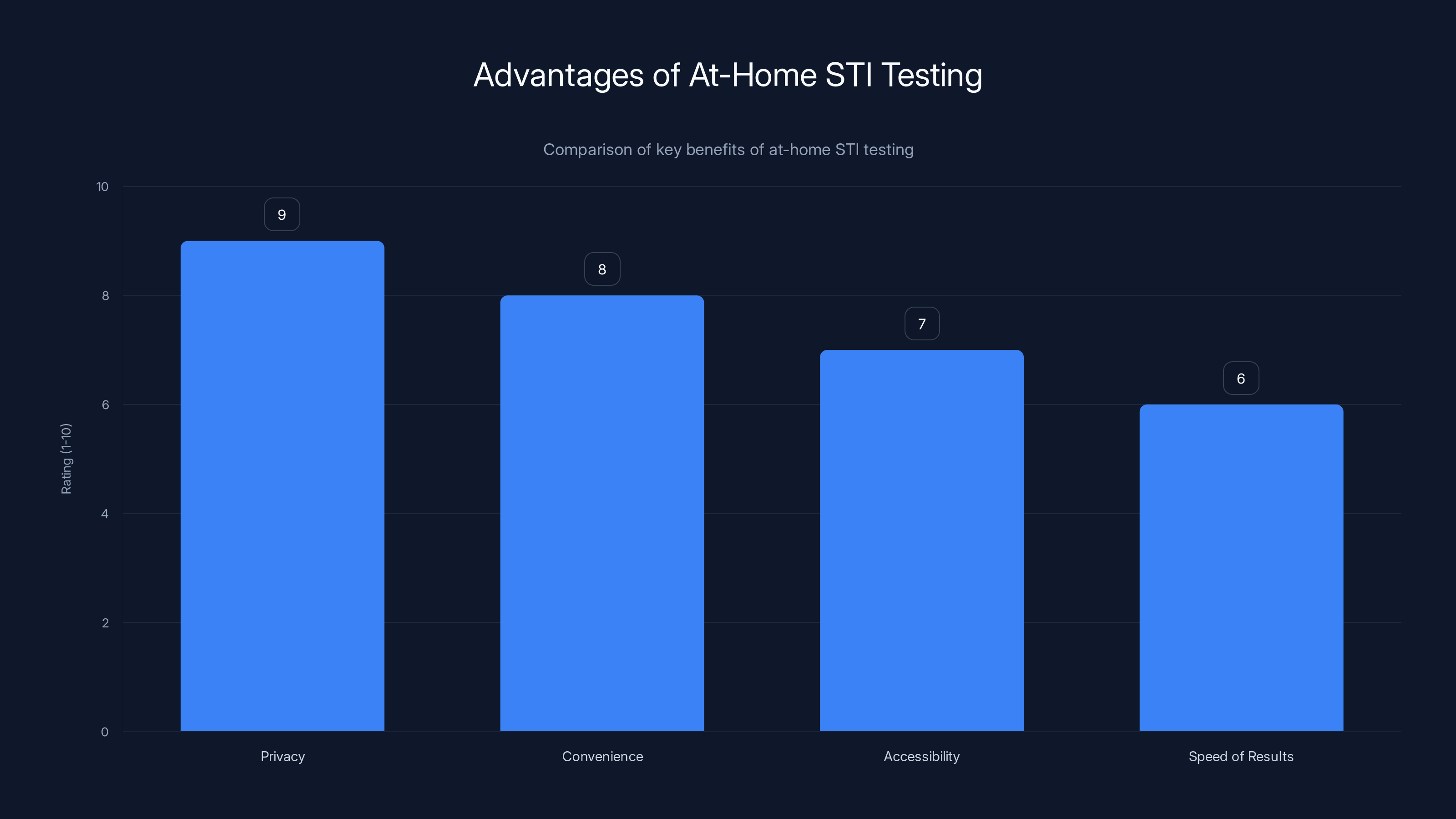
At-home STI testing offers significant advantages in privacy, convenience, accessibility, and speed, with privacy being the most highly rated benefit. Estimated data.
The Legitimate Disadvantages and Limitations
At-home STI testing isn't perfect, and honest assessment of downsides is essential for making good decisions.
Sample Collection Errors
The most common reason at-home STI tests fail is improper sample collection. You're not trained. You haven't collected hundreds of samples. You might not insert a swab far enough into the rectum or urethra. You might contaminate the sample with bacteria from your skin. You might not fill the urine collection cup to the line. These collection errors lead to false negatives—the test says you're negative when you're actually positive.
Clinic-based tests have lower error rates because trained professionals collect samples consistently. Studies show that roughly 5-10% of at-home STI tests are collected incorrectly, leading to roughly 5-10% false negative rates. That's not disastrous, but it means if you test negative at home after a high-risk encounter, there's a non-trivial chance you actually have an infection.
Limited Test Coverage
Not all at-home tests check for all STIs. Some screen for only chlamydia and gonorrhea. Others add syphilis. A few include trichomonas. But comprehensive tests that include HIV, herpes, hepatitis B, hepatitis C, and other infections? Those are rare and expensive. You might need multiple kits to get comprehensive coverage, which defeats the cost advantage.
Clinics can order comprehensive panels that test for everything with a single specimen. At-home testing is more limited by design.
Viral Infection Testing Reliability
As mentioned earlier, viral STI testing at home is less reliable than bacterial testing. Window periods for HIV extend weeks, herpes antibodies might not be detectable in asymptomatic people, and hepatitis antibodies take months to appear. A home test that comes back negative for HIV doesn't actually rule out infection if you tested too early. This false reassurance is dangerous because it might cause you to engage in risky behavior while unknowingly infectious.
Professional Follow-Up Required for Positives
Here's a critical reality: if you test positive, you're going to need to contact a medical professional anyway. You need prescription medication for chlamydia, gonorrhea, and syphilis. You need confirmation testing for HIV. You need counseling about sexual partners and transmission risk. The at-home test saves you one visit, but not all visits.
Some at-home test companies include telehealth consultations, which helps but isn't the same as a full clinic workup. If you have complicated medical history, pregnancy, allergies to antibiotics, or other considerations, at-home testing plus telehealth might not be enough.
No Symptoms Assessment
At-home tests can't assess your symptoms or examine you. Some STIs cause unique symptoms or complications that matter for treatment decisions. Pelvic inflammatory disease (PID) caused by chlamydia or gonorrhea requires more aggressive treatment than uncomplicated infection. Doctors can assess severity during physical examination. At-home testing can't replicate this.
Accuracy Still Requires Proper Timing
A negative result from an at-home test is only reliable if you tested at the right time after exposure. Most STIs aren't detectable for days or weeks after infection. If you test too early, you'll get a false negative. At-home testing doesn't include counseling about window periods the way professional testing does, potentially leading to dangerously false reassurance.
Comparison: At-Home vs. Clinic vs. Telehealth Testing
Let's break down how different testing approaches actually compare across key dimensions.
| Factor | At-Home | Clinic Visit | Telehealth | Pharmacy |
|---|---|---|---|---|
| Privacy | Excellent | Poor | Good | Fair |
| Cost | $100-400 | $50-200 (with insurance) | $75-150 | $100-350 |
| Speed of Results | 30 min - 5 days | 2-7 days | 2-7 days | Same-day to 5 days |
| Accuracy (Bacterial) | 95-98% | 98%+ | 98%+ | 95-98% |
| Accuracy (Viral) | 85-95% | 95%+ | 95%+ | 85-95% |
| Test Comprehensiveness | Limited | Comprehensive | Varies | Limited |
| Accessibility | Excellent | Poor (waiting lists) | Good | Moderate |
| Follow-up Available | Some kits | Yes | Yes | No |
| Professional Assessment | No | Yes | Limited | No |
| Good For Low-Risk Testing | Yes | Overkill | Yes | Yes |
| Good For High-Risk Testing | No | Yes | Maybe | No |
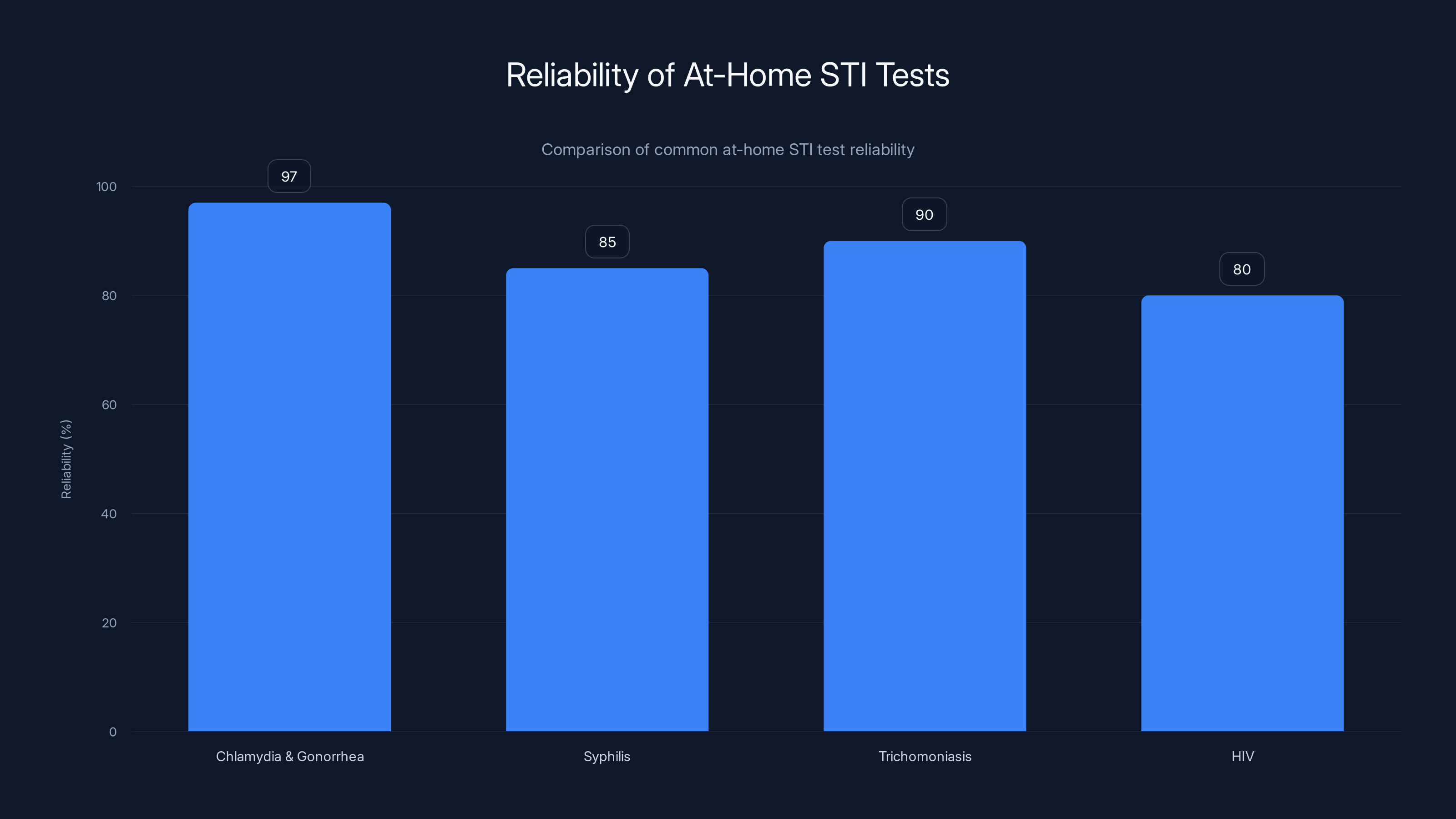
Chlamydia and Gonorrhea tests are the most reliable at-home STI tests with 97% accuracy. Syphilis and Trichomoniasis tests are less common and slightly less reliable, while HIV tests have the lowest reliability due to the window period. Estimated data.
Popular At-Home STI Test Options and What They Offer
The market now includes dozens of options. Here are the most credible and widely available.
Rapid PCR Tests (30-Minute Results)
Rapid PCR tests represent the newest category. They work like at-home COVID tests: you collect a sample, insert it into a tabletop device, and get results within 30 minutes. Everlywell's rapid STI test is the most prominent example. You collect a sample, the machine analyzes it using polymerase chain reaction (PCR) technology, and you get results on your phone.
The advantage is speed. You know your status same-day. The disadvantage is limited availability—these tests are primarily available for people with vaginas currently, and they test for three common STIs rather than comprehensive panels. Cost is typically $150-200 for rapid tests.
Mail-In Labs (5-Day Results)
Mail-in testing is the traditional at-home model. You collect samples (urine, swabs, or blood), seal them in a pre-paid mailer, send them to a certified laboratory, and get results in your app within 3-5 business days. Companies like Lets Get Checked, Everly Well, Wisp, and others offer mail-in testing.
Advantages include comprehensive testing options (some kits test for 5+ infections), lower costs ($100-150 for basic panels), and accessibility nationwide. Disadvantages include slower results, higher collection error rates, and no results while waiting. Many include telehealth follow-up if you test positive.
Specialty Options: Sex Toy Companies
Dame, a sex toy maker, now offers at-home STI testing kits. The tests are reliable—they use certified labs and NAAT technology—but the marketing angle is novel: testing positioned specifically for people with vaginas, with options for three-site testing (urine, vaginal swab, and oral/rectal samples simultaneously).
The value proposition is less about the test itself and more about brands taking sexual health seriously. Cost is comparable to other kits ($150-200), but some people appreciate the positioning from a sexuality-positive company.
Pharmacy-Based Options
Walgreens, CVS, and other major pharmacies now stock at-home STI test kits. These are typically rapid tests or mail-in options from established brands. The advantage is immediate availability—no shipping delay. The disadvantage is less privacy (someone might see you buying it at the pharmacy, though you can order online for pickup).

Understanding Accuracy: What the Data Actually Shows
Accuracy is the most important question. Do these tests actually work?
For bacterial infections like chlamydia and gonorrhea, the answer is yes. Studies consistently show 95-98% sensitivity (correctly identifying positive cases) and 97-99% specificity (correctly identifying negative cases) for at-home NAAT tests. This matches clinic-based testing accuracy.
However—and this is critical—accuracy depends entirely on proper collection. Studies showing 95%+ accuracy enrolled participants and provided careful instruction. Real-world accuracy among people who just followed the instructions in the box is probably 5-10% lower due to collection errors.
For viral infections, accuracy is lower. HIV home tests show 92-99% sensitivity depending on the specific test, but many fail during window periods (the first 18-45 days after infection when antibodies haven't developed yet). Herpes home tests are even less reliable for asymptomatic people because antibody levels might be below detection thresholds.
The research is clear: at-home testing works well for bacterial infections when samples are collected properly, adequately for viral infections with appropriate caveats about timing, and is less suitable for comprehensive screening compared to clinic-based testing.
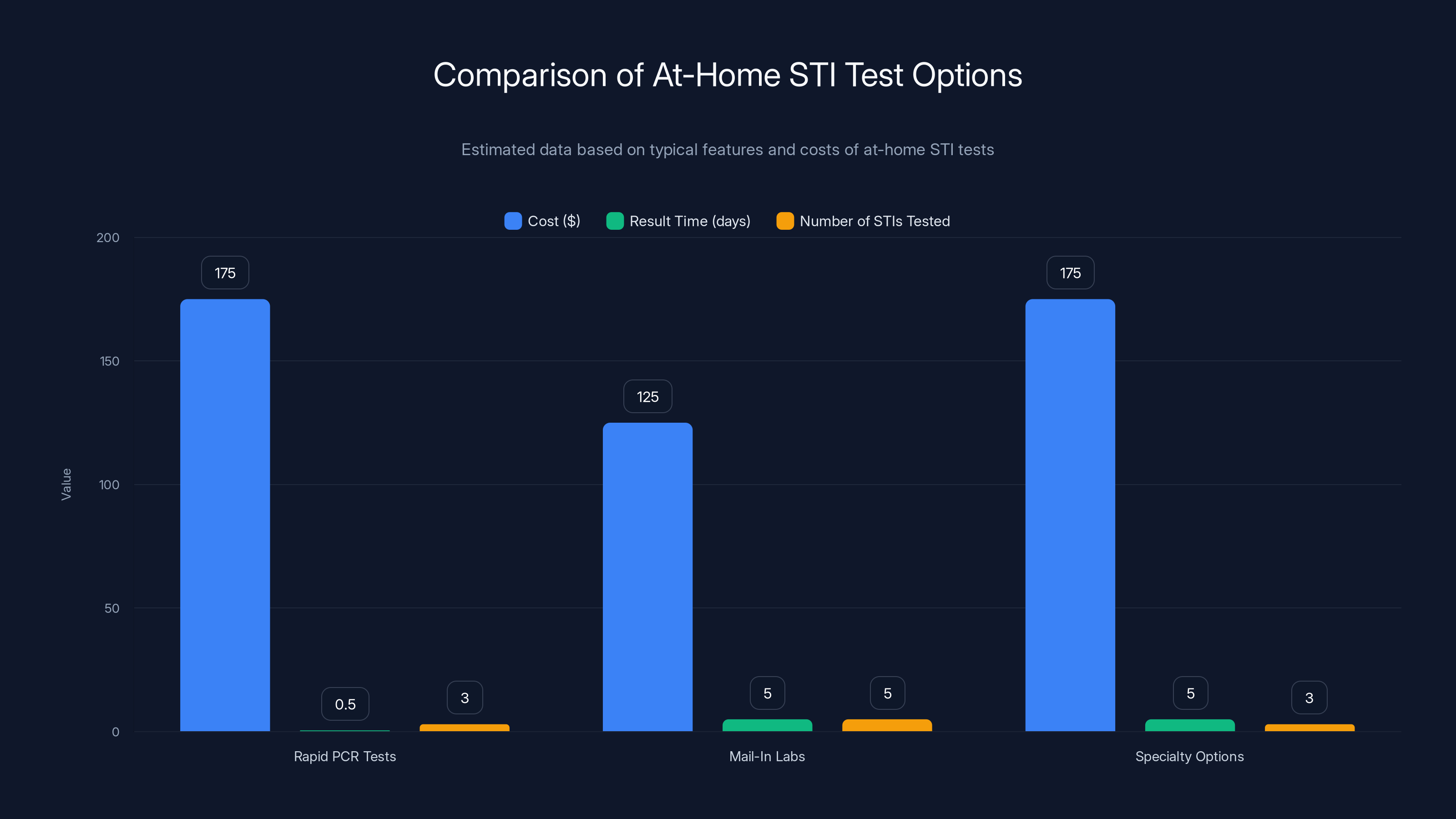
Rapid PCR tests offer the fastest results but test for fewer STIs. Mail-in labs provide comprehensive testing at a lower cost, while specialty options focus on specific demographics. Estimated data based on typical features.
The Cost-Benefit Analysis: When At-Home Testing Makes Sense
At-home STI testing makes sense in specific scenarios, not universally.
When to Choose At-Home Testing
You should use at-home testing if:
- You're a low-risk individual (monogamous, stable relationship, previous negative tests) doing routine screening
- You're recently single and want to test before new sexual partners
- You have barriers to clinic access (rural location, no transportation, inflexible work schedule)
- You have anxiety in medical settings that prevents you from getting tested otherwise
- You're uninsured or underinsured and can't afford clinic testing
- You value privacy highly and won't test otherwise
- You specifically want rapid results (for recent-exposure scenarios)
When to Skip At-Home Testing
You should absolutely use clinic-based testing if:
- You're at high risk of infection (multiple partners, inconsistent condom use, partner with unknown status, recent condom failure)
- You have symptoms (unusual discharge, pain, ulcers, rashes)
- You had a specific potential exposure and need accurate testing with proper window-period counseling
- You need comprehensive testing beyond the 2-4 STIs covered by most at-home kits
- You need professional assessment (pregnancy, complex medical history, allergies)
- You're HIV-positive and need viral load monitoring
- You need sexual health counseling, partner notification, or other professional services
Think of at-home testing as a screening tool for low-risk, asymptomatic individuals. Think of clinic testing as the comprehensive option for everyone else.

Positive Results: What Happens Next?
If your at-home test comes back positive, panic is understandable but unnecessary. Virtually all bacterial STIs are easily curable with antibiotics. Viral infections are manageable with modern treatment.
Your immediate next steps depend on what test you used. Most kits provide a telehealth consultation within 24-48 hours. A provider will discuss treatment options, potentially write a prescription (many telehealth services can prescribe antibiotics remotely), and counsel you about notification of sexual partners.
For bacterial infections, treatment is straightforward: antibiotics (often azithromycin or doxycycline) taken for 7-10 days, follow-up testing if recommended, and partner notification. For viral infections like HIV, you need confirmation testing and may need to start antiretroviral therapy, requiring an infectious disease specialist.
One critical point: notification of partners is ethically essential but fraught with complexity. Some partners appreciate direct notification. Others don't want contact. Providers can help navigate this delicate conversation.

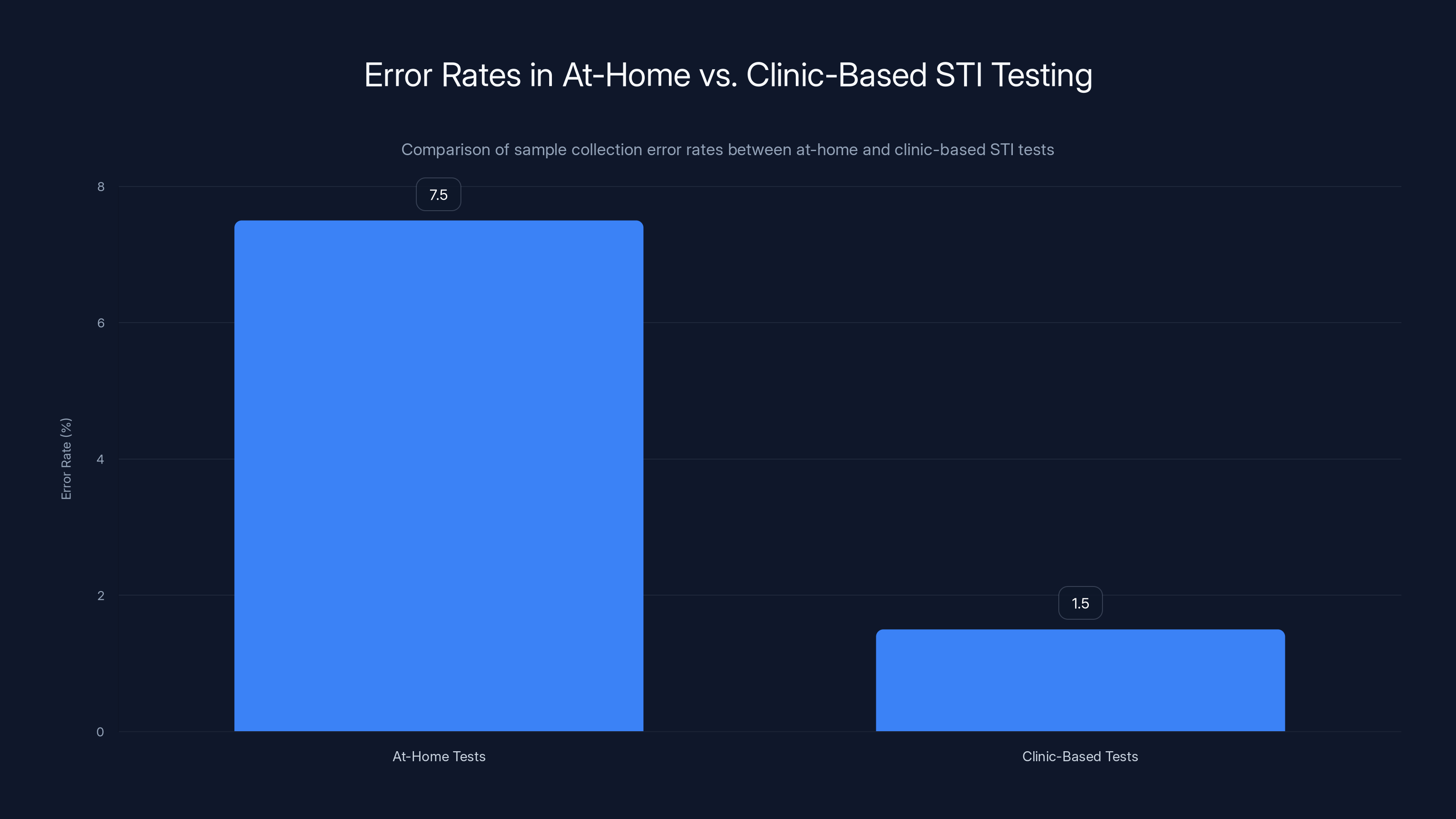
At-home STI tests have an estimated error rate of 5-10%, averaging around 7.5%, compared to 1.5% for clinic-based tests, highlighting the importance of professional sample collection.
Negative Results: Why False Negatives Matter
A negative result is reassuring but not absolute proof of non-infection. False negatives happen for three reasons:
First, collection errors. You didn't collect the sample properly, contaminated it, or didn't test the right site. Swabbing the wrong location or inserting a swab insufficiently are common errors that produce false negatives.
Second, timing. You tested during the window period before the infection was detectable. If you tested three days after exposure for chlamydia, which has a detection window of 7+ days, you'll test negative despite being infected.
Third, infection location. If you have a throat infection but only tested urine, you'll test negative. Multi-site testing reduces this risk but requires correct collection at each site.
For this reason, negative results should be interpreted with context. If you had a specific high-risk exposure, a single negative test isn't dispositive. Retesting after the appropriate window period is prudent.

Sexual Health Responsibility Beyond Testing
At-home STI testing is one piece of sexual health, not the entire picture.
Prevention Still Matters Most
Testing catches infections that prevention fails to stop. But prevention should be the first line. Consistent condom use prevents 95%+ of STI transmission. Regular conversations about sexual history and health status prevent misunderstandings. Vaccination prevents HPV and hepatitis B.
At-home testing enables regular screening, which is important, but shouldn't replace prevention efforts.
Partner Communication
Responsible sexual health includes honest communication with partners. Before sexual activity, discussing STI status (based on recent testing), current preventive practices, and monogamy expectations is essential. At-home testing makes frequent screening possible, but only if you actually tell partners about the results.
Open Access to Medical Care
At-home testing should complement, not replace, access to comprehensive sexual health care. That includes gynecological exams, discussions of contraception, assessment of sexual dysfunction or concerns, and counseling. Even if at-home testing is negative, annual sexual health checkups are valuable.

The Future of At-Home STI Testing
Expect this category to expand significantly over the next few years.
Multiplex Testing
Future tests will simultaneously detect 6-10+ STIs from single samples, approaching the comprehensiveness of clinic testing. Technological advances in molecular biology are making this feasible.
Faster Results
As rapid PCR technology becomes more affordable, 30-minute results will become standard rather than exceptional, closing the speed gap between at-home and professional testing.
Better Integration
At-home tests will increasingly include professional consultation, sexual health education, partner notification assistance, and follow-up monitoring. The boundary between "at-home" and "telehealth" will blur.
Precision Medicine
Genetic testing combined with STI testing might predict who's at highest risk, enabling preventive treatment for high-risk individuals who haven't contracted infections yet. This is speculative but technically feasible.

Recommendations: Who Should Test and How Often
Based on current evidence, here are practical recommendations.
Annual screening is appropriate for anyone sexually active with any partner whose status isn't completely known. This includes people in monogamous relationships with new partners, people with multiple partners, and anyone not fully vaccinated for HPV and hepatitis B.
More frequent testing (every 3-6 months) makes sense for people with multiple partners, people with partners of unknown status, or anyone in high-prevalence sexual networks.
Testing after specific exposures (condom failure, new partner, partner disclosure of infection) should happen after appropriate window periods, usually 5-7 days for bacterial infections.
Comprehensive professional testing should happen at least once in your life to establish baseline sexual health, assess for infections you might not suspect, and discuss preventive strategies with a qualified provider.

Common Questions About At-Home STI Testing
Can I test too soon after exposure?
Yes. Most STIs have "window periods" where they're not yet detectable. Chlamydia and gonorrhea become detectable 5-7 days after infection. HIV takes 18-45 days depending on the test type. Testing during window periods produces false negatives that give dangerous false reassurance. If you test immediately after a high-risk encounter, retesting after the appropriate window period is necessary.
What if my test is inconclusive?
Some tests return inconclusive or invalid results if the sample was inadequate. Most companies will send replacement tests if this happens. Inconclusive results should be repeated with careful attention to collection instructions.
Do insurance plans cover at-home STI tests?
Maybe. Many plans cover STI testing, but may require clinic-based testing. Some specifically cover at-home testing. Check your plan details or call your insurer before purchasing. If covered, at-home tests might be free or require a copay.
Can I test while on antibiotics if I'm being treated?
No. Antibiotics kill the bacteria being tested for, producing false negatives. Wait until you've completed treatment and the recommended follow-up testing period (usually 2-4 weeks) before retesting with at-home kits.
Is at-home testing okay during pregnancy?
Most at-home tests are safe during pregnancy since you're just collecting samples. However, some antibiotics used to treat STIs aren't safe in pregnancy. For this reason, pregnant people should use clinic-based testing where providers can assess for pregnancy and prescribe pregnancy-safe treatments. This is one clear scenario where at-home testing is inadequate.
Do results get shared with partners automatically?
No. At-home testing is confidential. Your results are yours. Partner notification is entirely up to you. Most providers can help facilitate partner notification if you're uncomfortable doing it yourself, but nothing is automatic.
Conclusion: At-Home STI Testing Is Here to Stay
At-home STI testing has fundamentally changed sexual health screening. For the first time, people can be tested without embarrassment, without appointments, without time off work, and often at lower cost than traditional clinic testing.
The technology works. Accuracy for bacterial infections rivals professional testing. Speed is competitive. Privacy is excellent. For low-risk individuals doing routine screening, at-home testing is entirely reasonable.
But at-home testing isn't a replacement for comprehensive sexual health care. It's one tool among many. For people with symptoms, high-risk exposures, or complex medical histories, professional testing is essential. For comprehensive sexual health—which includes contraception discussions, gynecological exams, sexual dysfunction assessment, and prevention counseling—clinic care remains irreplaceable.
The best approach is probably layered: use at-home testing for regular screening and peace of mind, but maintain access to comprehensive sexual health care through a trusted provider. Test frequently enough that you know your status with confidence. Communicate honestly with partners. Prevent infections whenever possible through vaccination, barrier methods, and honest conversations.
STI testing shouldn't be embarrassing or burdensome. For many people, at-home testing has removed the barriers that prevented them from testing at all. If at-home testing increases the number of people who know their sexual health status, that's an unambiguous public health victory.
Your sexual health matters. Testing—whether at home, at a clinic, or through telehealth—is how you protect yourself and your partners. Stop avoiding it. The process has gotten easier.

FAQ
What is an at-home STI test?
An at-home STI test is a self-administered diagnostic kit that uses samples you collect yourself (urine, swabs, or blood) to detect sexually transmitted infections. You either process samples in a device at home that provides results within 30 minutes, or seal samples in a pre-paid envelope and mail them to a certified laboratory for results within 3-5 business days. The tests use the same laboratory technology as clinic-based testing, including NAAT and PCR methods.
How accurate are at-home STI tests compared to professional testing?
For bacterial infections like chlamydia and gonorrhea, at-home tests are 95-98% accurate when samples are collected properly, matching professional clinic accuracy. Accuracy depends heavily on following collection instructions correctly. For viral infections like HIV and herpes, accuracy is lower (85-95%) and depends on testing at the right time after exposure, since these infections have window periods before they're detectable. Real-world accuracy is typically 5-10% lower than laboratory studies because collection errors happen outside controlled research settings.
Should I test at home if I have symptoms?
No. If you have unusual discharge, pelvic pain, urethral pain, sore throat, rectal pain, or other symptoms potentially indicating STI, see a healthcare professional rather than using at-home testing. Healthcare professionals can assess symptoms, examine you, evaluate for complications, and consider alternative diagnoses. At-home testing can't replace physical examination and professional assessment.
What should I do if I get a positive result?
If you test positive, contact the telehealth provider usually included with your test kit within 24 hours. Most providers can prescribe antibiotics for bacterial infections immediately. You'll discuss treatment options, potential side effects, partner notification, and follow-up testing. For viral infections like HIV, you need confirmation testing and may need to see a specialist. The key point: a positive at-home result means you contact a professional—at-home testing doesn't end the process, it starts it.
How often should I test for STIs?
The CDC recommends annual screening for anyone sexually active. If you have multiple partners, partners of unknown status, or a partner who has other partners, testing every 3-6 months is prudent. If you've had a specific high-risk exposure (condom failure, new partner), test after appropriate window periods (5-7 days for bacterial infections, 18-45 days for HIV). One-time testing is insufficient—your status can change with each new partnership, so regular screening is essential.
Are at-home STI tests covered by insurance?
Sometimes. Some insurance plans cover STI testing but may require clinic-based testing. Others specifically cover at-home tests. Check your plan's coverage details or call your insurer before purchasing. Even if at-home tests aren't covered, they're often FSA or HSA-eligible, meaning you can use pre-tax dollars to purchase them, reducing effective cost by 20-30% depending on your tax bracket.
What's the difference between window period and incubation period?
The window period is the time between infection and when tests can detect it—roughly 5-7 days for bacterial infections and 18-45 days for HIV. The incubation period is when you have the infection but don't yet have symptoms—sometimes weeks or months. You can test positive before developing any symptoms, which is why regular screening matters. Testing too early (during the window period) produces false negatives.
Can I do at-home STI testing while pregnant?
Sample collection is safe, but treatment is complicated. Many antibiotics used for bacterial STI treatment aren't safe during pregnancy. If you're pregnant, use professional clinic testing where providers can prescribe pregnancy-safe antibiotics and monitor treatment. This is one clear scenario where at-home testing is inadequate because it lacks professional guidance on safe treatment options.

Key Takeaways
- At-home STI tests provide accurate detection for bacterial infections like chlamydia and gonorrhea when samples are collected properly, making them viable alternatives to clinic testing for routine screening
- Rapid PCR tests deliver results in 30 minutes while mail-in tests take 3-5 days; choose based on how quickly you need results
- Viral infection testing (HIV, herpes, hepatitis) is less reliable at home due to window periods and antibody detection limitations, making professional testing preferable if viral infection is suspected
- Cost ranges from $100-400 depending on test comprehensiveness, and most are FSA/HSA-eligible, potentially reducing effective cost through pre-tax purchasing
- Privacy, accessibility, and convenience make at-home testing appealing for low-risk individuals, but symptoms, high-risk exposures, or complex medical situations require professional evaluation
- Positive results still require professional follow-up for treatment prescription and partner notification guidance; at-home testing starts the process rather than ending it
- Regular testing (annually for all sexually active people, every 3-6 months for higher-risk individuals) is essential since sexual health status changes with new partners

![At-Home STI Tests: Complete Guide to Pros, Cons & Best Options [2026]](https://tryrunable.com/blog/at-home-sti-tests-complete-guide-to-pros-cons-best-options-2/image-1-1771763732419.png)



