The Measles Outbreak in Idaho: Understanding the Risks and the Path Forward [2025]
When measles found its way onto a plane bound for Idaho, it didn't just bring an infectious virus into a state with the worst vaccination rates in the country—it raised alarms about public health, policy, and the future of disease prevention in the United States. As we delve into this complex issue, let's explore the implications, challenges, and opportunities for improvement.
TL; DR
- Idaho's measles vaccination rate is the lowest in the U.S., with only 78.5% of kindergartners vaccinated, according to CDC data.
- Measles exposure occurred at Boise airport on March 29, potentially affecting many travelers, as reported by Idaho News.
- Symptoms of measles include fever, cough, runny nose, and red eyes, appearing 7-21 days after exposure, detailed by CDC.
- Vaccination is key to preventing outbreaks, yet misinformation and policy gaps persist, as discussed in Britannica.
- Future trends suggest increased focus on community outreach and education, as highlighted by The New York Times.
- Practical steps include improving access and addressing vaccine hesitancy, as suggested by KFF.
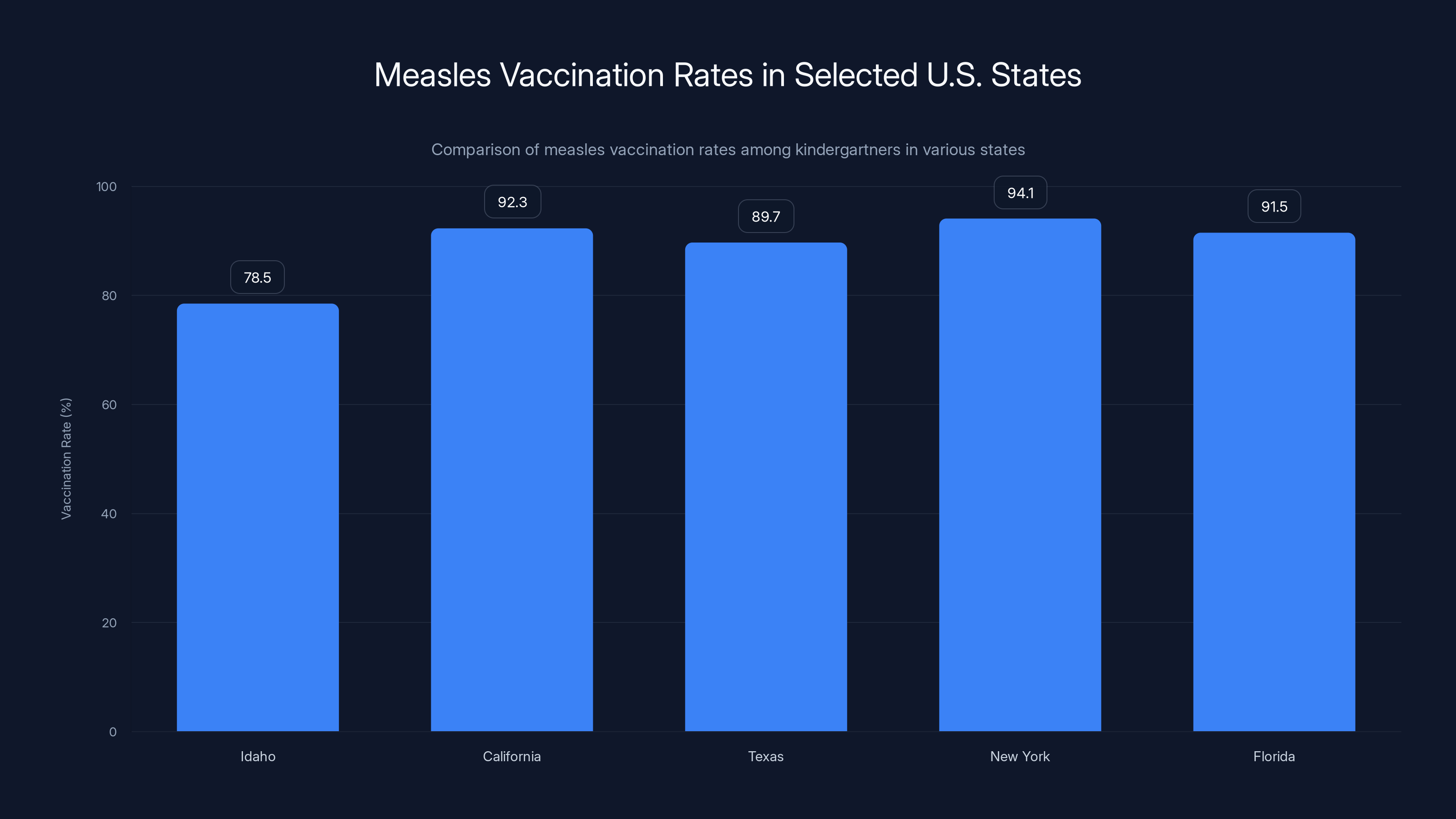
Idaho has the lowest measles vaccination rate among kindergartners at 78.5%, highlighting the need for improved vaccination efforts. Estimated data for other states.
Introduction
Last month, an individual carrying the measles virus passed through Boise airport, Idaho's busiest hub. This event has reignited concerns about the state's vaccination rates, which are the lowest in the nation. With only 78.5% of kindergartners vaccinated against measles, Idaho is vulnerable to outbreaks that could have been easily prevented with higher vaccination coverage, as noted by the CDC.
The Reality of Measles
Measles is not just another childhood illness—it's highly contagious and can lead to severe complications, especially in young children and immunocompromised individuals. The virus is spread through respiratory droplets, making it incredibly easy to transmit in crowded spaces like airports, as explained by UCHealth.
Understanding Measles Transmission
Measles is one of the most contagious viruses known. Here's how it spreads:
- Airborne Transmission: When an infected person coughs or sneezes, the virus can remain in the air for up to two hours.
- Contact Transmission: Touching a contaminated surface and then touching the face can lead to infection.

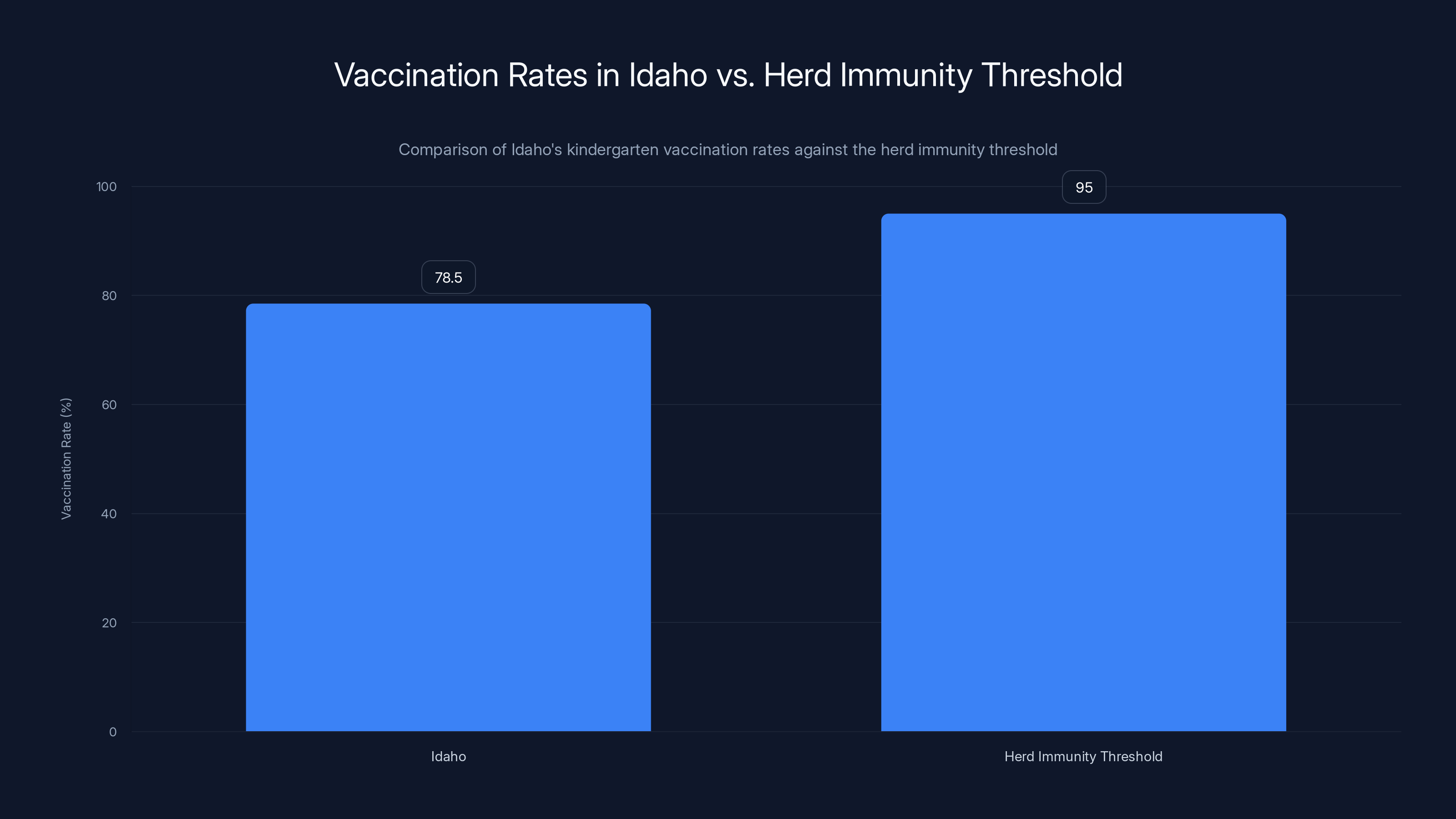
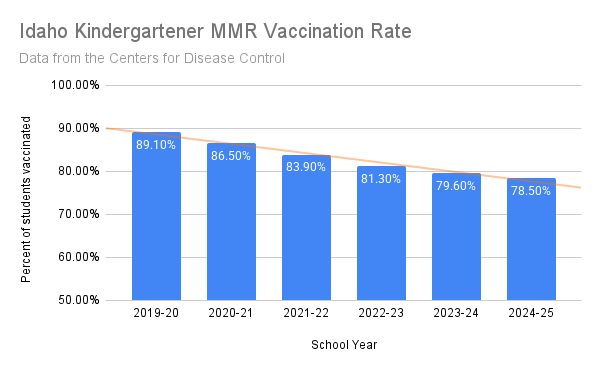
Idaho's kindergarten vaccination rate is 78.5%, significantly below the 95% herd immunity threshold, increasing the risk of outbreaks.
Idaho's Vaccination Landscape
Idaho's vaccination rates are a concern. With only 78.5% of kindergartners vaccinated, the state falls below the herd immunity threshold of 95% necessary to prevent outbreaks, as highlighted by CDC research.
Factors Contributing to Low Vaccination Rates
Several factors contribute to Idaho's low vaccination rates:
- Vaccine Hesitancy: Misinformation about vaccine safety and efficacy.
- Policy Gaps: Lack of mandates and easy opt-out options for parents, as discussed in Britannica.
- Access Issues: Rural areas with limited healthcare facilities.
The Impact of Measles Outbreaks
Outbreaks of measles have far-reaching impacts, not only on public health but also on economic stability and social structures.
Health Implications
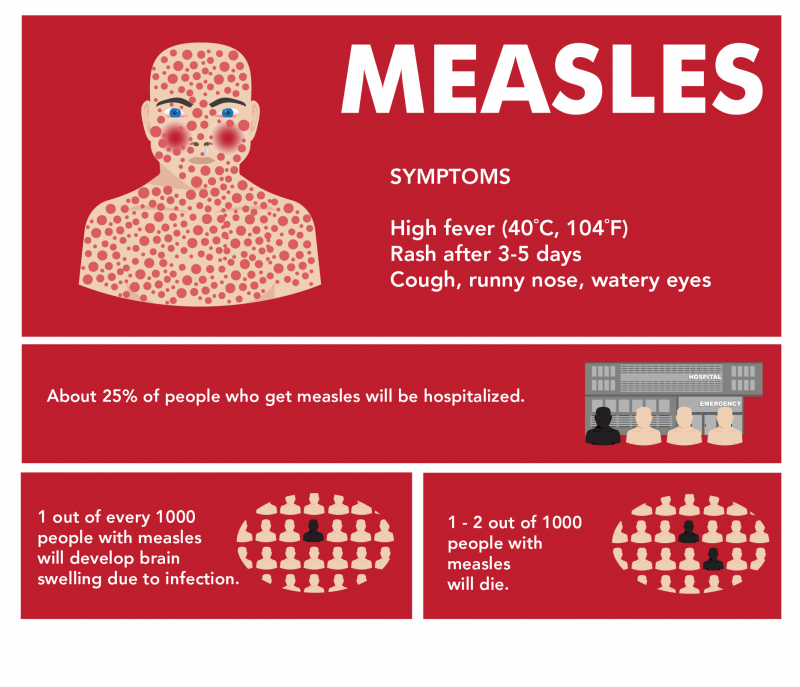
Measles can lead to severe health complications, including:
- Pneumonia: The most common cause of death in measles outbreaks.
- Encephalitis: Swelling of the brain that can lead to seizures or permanent brain damage.
- Subacute Sclerosing Panencephalitis (SSPE): A rare but fatal brain disorder that can occur years after infection.
Economic and Social Consequences
The economic burden of a measles outbreak includes healthcare costs and lost productivity:
- Healthcare Costs: Hospitalizations and treatments can strain local healthcare systems.
- Productivity Loss: Parents miss work to care for sick children, impacting family income.
- Social Disruption: School closures and quarantines can disrupt education and community activities.
The Role of Vaccination
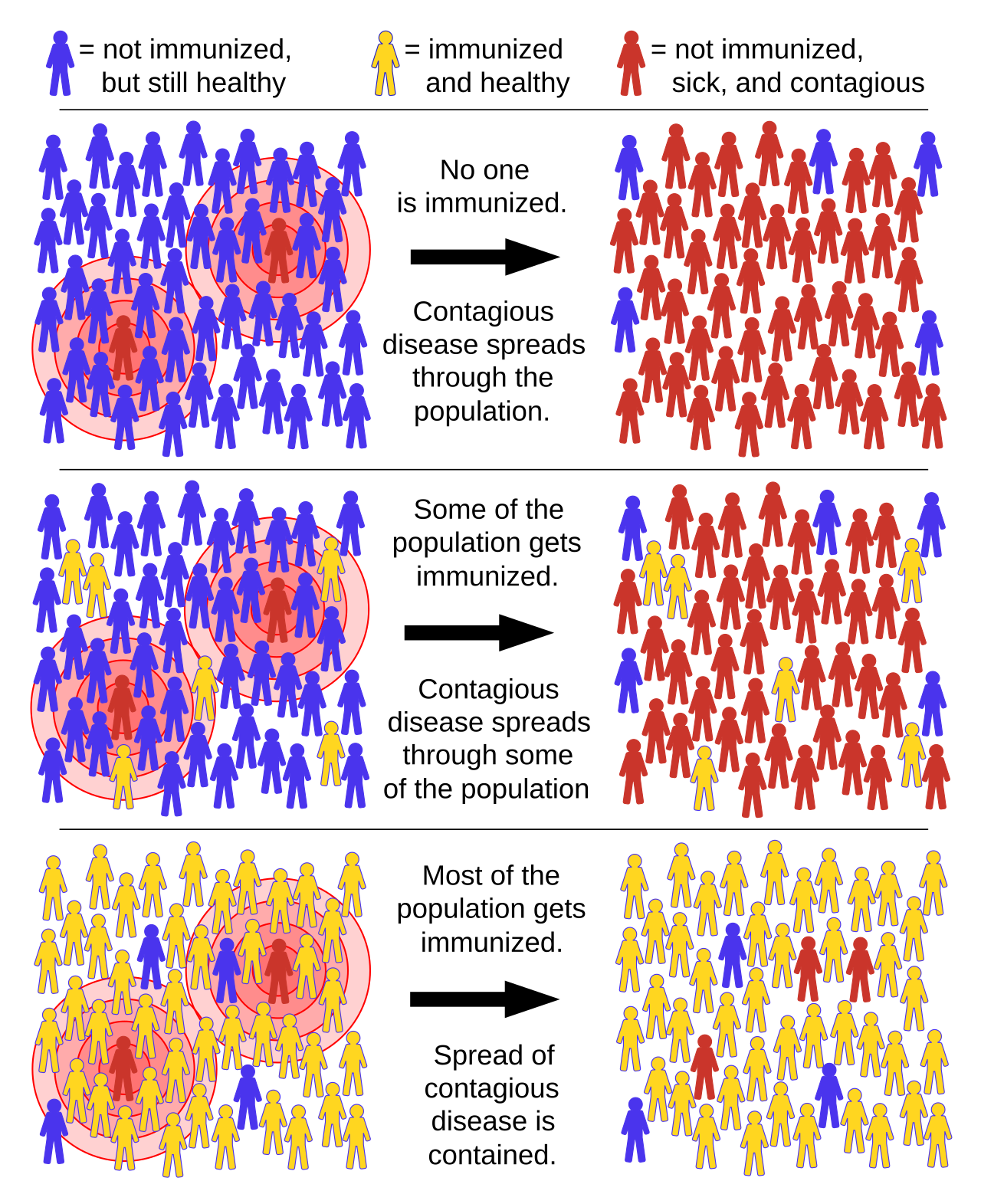
Vaccination remains the most effective way to prevent measles outbreaks. It's not just about individual protection, but community-wide immunity.
Benefits of Vaccination
- Herd Immunity: Protects those who cannot be vaccinated, such as infants and those with medical conditions.
- Prevention of Epidemics: High vaccination rates can prevent the spread of measles.
- Cost-Effectiveness: Reduces the need for expensive treatments and hospitalizations, as emphasized by CDC.
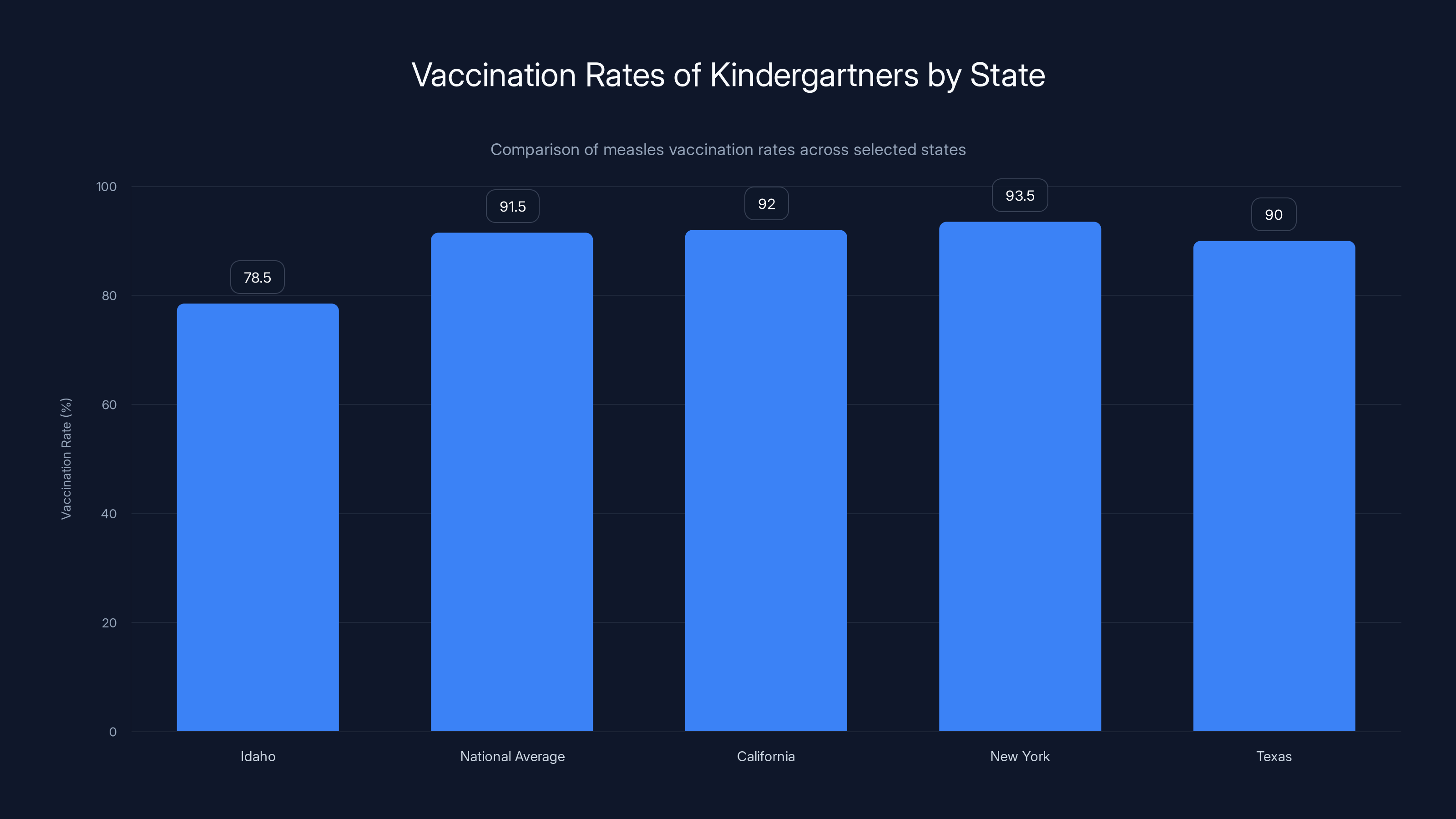
Idaho has the lowest measles vaccination rate among kindergartners at 78.5%, significantly below the national average of 91.5%.
Overcoming Vaccine Hesitancy
Addressing vaccine hesitancy is critical to improving vaccination rates. This involves tackling misinformation and building trust in vaccines.
Strategies to Combat Hesitancy
- Education Campaigns: Clear, fact-based information about vaccine safety and benefits.
- Community Engagement: Involving local leaders to advocate for vaccination.
- Healthcare Provider Influence: Training providers to communicate effectively about vaccines, as suggested by The New York Times.
Policy Recommendations
Policy changes can significantly impact vaccination rates. Here are some recommendations:
- Mandatory Vaccination: Implement policies that require vaccination for school entry, with limited exemptions.
- Improved Access: Increase the availability of vaccines in rural and underserved areas.
- Data Monitoring: Use data to identify low-coverage areas and target interventions, as discussed by KFF.
Practical Implementation Guides
Implementing these recommendations requires a coordinated effort:
- Assess Local Needs: Identify areas with low vaccination coverage and understand the barriers.
- Develop Targeted Campaigns: Tailor messages to address specific community concerns.
- Enhance Provider Training: Equip healthcare workers with tools to address hesitancy.
- Monitor Progress: Use data to track improvements and adjust strategies as needed.
Common Pitfalls and Solutions
Pitfall: Misinformation
Solution: Use trusted voices and platforms to disseminate accurate information.
Pitfall: Policy Resistance
Solution: Engage stakeholders early in the policy development process to build consensus.
Pitfall: Access Barriers
Solution: Partner with local organizations to provide mobile vaccination clinics in underserved areas.
Future Trends and Recommendations
Looking ahead, several trends could impact vaccination efforts:
- Digital Health Tools: Utilizing technology to track vaccinations and send reminders, as noted in ReliefWeb.
- Personalized Health Communication: Tailoring messages to individual beliefs and concerns.
- Global Collaboration: Sharing strategies and data across borders to improve global health outcomes.
Conclusion
The measles outbreak in Idaho serves as a stark reminder of the importance of vaccination. By understanding the risks, challenges, and solutions, we can work towards a future where vaccine-preventable diseases are a thing of the past.
FAQ
What is measles?
Measles is a highly contagious viral infection that primarily affects children. It spreads through respiratory droplets and can lead to serious health complications, as outlined by CDC.
How does measles spread?
Measles spreads through the air when an infected person coughs or sneezes. The virus can remain viable in the air for up to two hours.
What are the benefits of measles vaccination?
Vaccination prevents the spread of measles, protects the community through herd immunity, and reduces healthcare costs by preventing illness.
What should I do if I'm exposed to measles?
If exposed, monitor for symptoms like fever, cough, and rash. Contact a healthcare provider for advice and potential post-exposure prophylaxis.
How can we improve vaccination rates?
Improving rates involves education, policy changes, and increasing access to vaccines, particularly in underserved areas.
Why is Idaho's vaccination rate so low?
Idaho's low rates are due to vaccine hesitancy, easy opt-out policies, and access issues in rural areas.
What are the symptoms of measles?
Symptoms include fever, cough, runny nose, red eyes, and a rash that spreads over the body.
Is there a cure for measles?
There is no specific cure for measles, but symptoms can be managed with supportive care. Vaccination is the best prevention.
Key Takeaways
- Idaho's vaccination rate is the lowest in the US, posing a high risk for measles outbreaks.
- Vaccination is critical for preventing measles and achieving herd immunity.
- Misinformation and policy gaps are major barriers to improving vaccination rates.
- Targeted education and community engagement can help overcome vaccine hesitancy.
- Future trends include digital health tools and personalized health communication.
- Policy changes are needed to mandate vaccinations and improve access in underserved areas.
- Monitoring and data-driven strategies are essential for tracking vaccination progress.
Related Articles
- Measles Resurgence: A Grim Warning for Future Pandemics [2025]
- CDC Leadership Crisis: The Ongoing Instability Threatening Public Health [2025]
- The Fallout of Robert Malone's Resignation from the CDC Vaccine Panel [2025]
- How the Shingles Virus Affects Aging: Unraveling the Mystery [2025]
- AI in Epidemiology: How ChatGPT Could Transform Outbreak Investigations [2025]
- Shingles Unveiled: Understanding and Managing the Silent Epidemic [2025]
![The Measles Outbreak in Idaho: Understanding the Risks and the Path Forward [2025]](https://tryrunable.com/blog/the-measles-outbreak-in-idaho-understanding-the-risks-and-th/image-1-1776117831064.jpg)



