The Shift Towards Shared Decision-Making in Vaccine Policy: A Comprehensive Guide [2025]
In recent years, the healthcare landscape has seen significant shifts, particularly in the realm of vaccine policy. The concept of shared decision-making has gained traction, spearheaded by influential figures like US Health and Human Services Secretary Robert F. Kennedy Jr. This article delves into the intricacies of shared decision-making in the context of vaccines, exploring its implications, practical applications, and future outlook.
TL; DR
- Shared Decision-Making: Empowers patients by involving them in healthcare decisions, balancing medical expertise with personal values.
- Practical Implementation: Involves clear communication, understanding patient concerns, and providing evidence-based options.
- Challenges: Includes potential misinformation, varying patient literacy levels, and time constraints in clinical settings.
- Technological Integration: AI tools and digital platforms can enhance shared decision-making processes.
- Future Trends: Anticipates wider adoption, policy adjustments, and increased role of technology in patient-provider interactions.

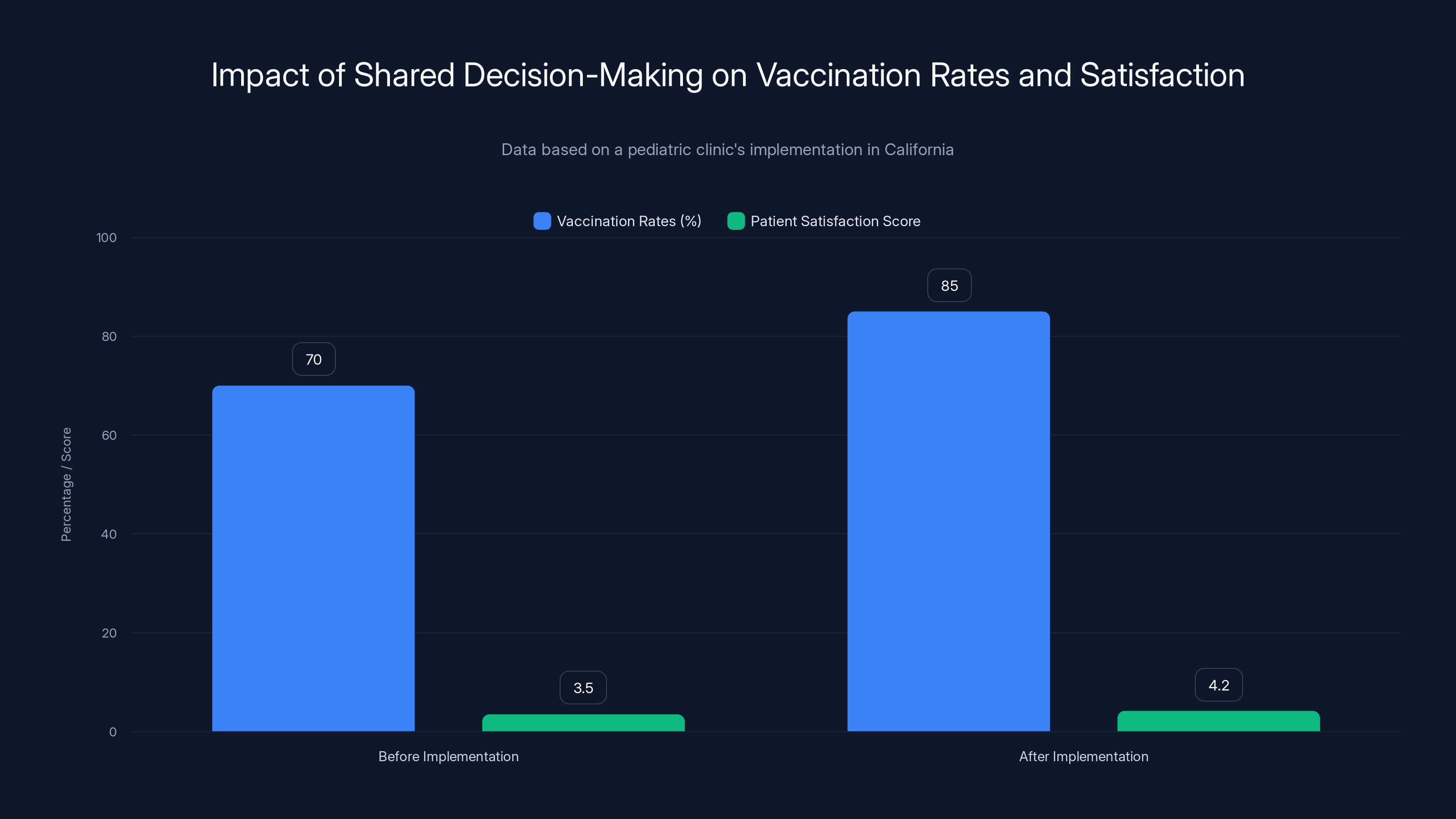
The introduction of shared decision-making in a pediatric clinic led to a 15% increase in vaccination rates and a notable improvement in patient satisfaction scores. Estimated data for satisfaction scores.
Understanding Shared Decision-Making
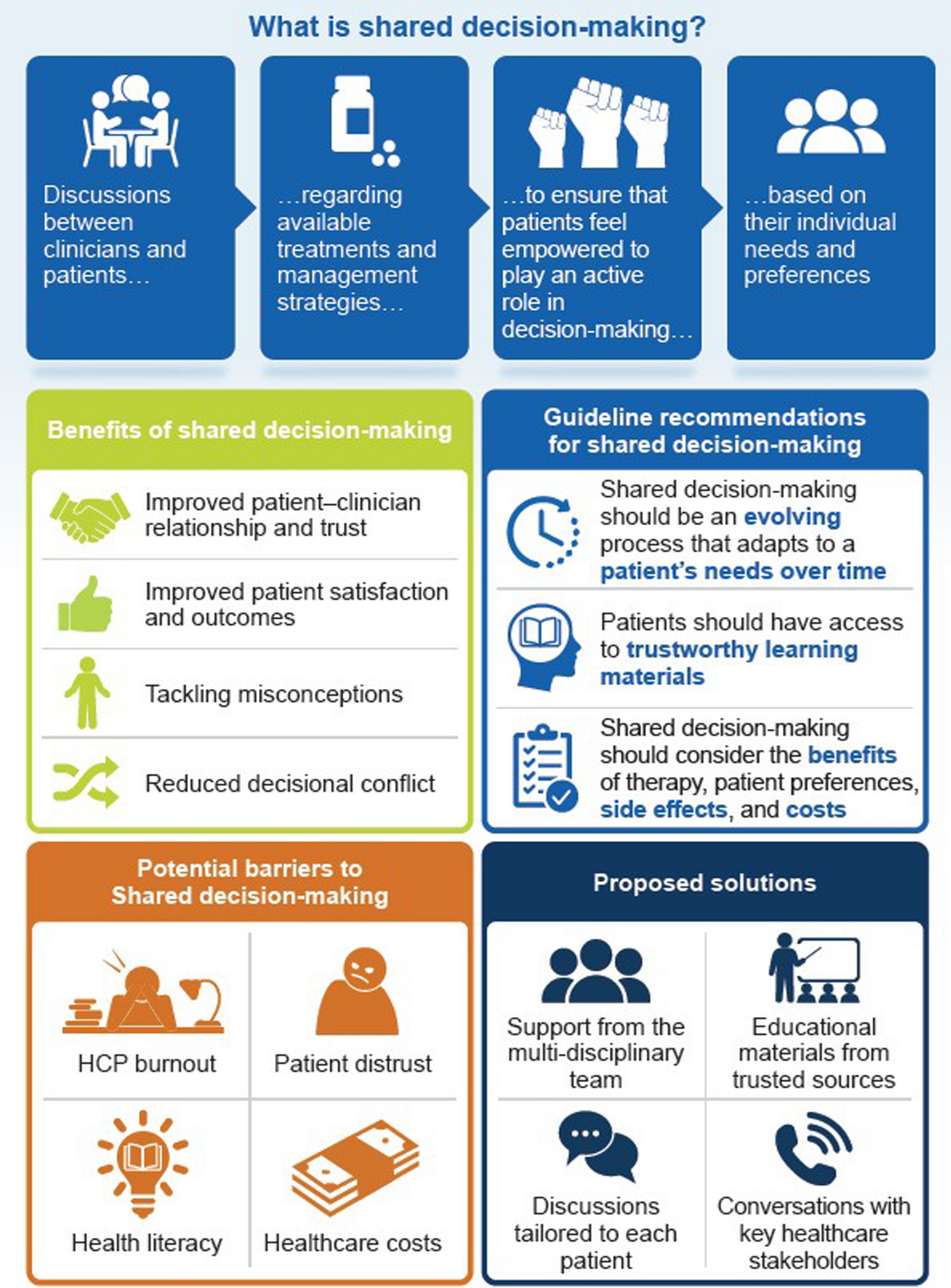
Shared decision-making (SDM) is a collaborative process that allows patients and healthcare providers to make healthcare decisions together. This approach considers the best scientific evidence available, as well as the patient's values and preferences. The goal is to empower patients by involving them in the decision-making process, rather than having healthcare decisions solely dictated by medical professionals.
Historical Context
Historically, healthcare decisions were predominantly made by medical professionals, with patients playing a passive role. The shift towards shared decision-making began gaining momentum in the late 20th century, driven by a growing recognition of patient autonomy and the importance of personalized care.
The Role of RFK’s CDC
Under the leadership of Robert F. Kennedy Jr., the Centers for Disease Control and Prevention (CDC) has embraced shared decision-making, particularly in the context of vaccine policy. This shift reflects a broader movement towards patient-centered care, where individual preferences and circumstances are considered alongside clinical guidelines.


Projected improvements in patient satisfaction and health outcomes due to decision aids are estimated at 20%, with technology integration potentially enhancing shared decision-making by 25%. Estimated data.
Practical Implementation of Shared Decision-Making
Implementing shared decision-making in clinical practice involves several key steps:
- Creating a Supportive Environment: Healthcare settings must foster an atmosphere where patients feel comfortable expressing their concerns and preferences.
- Effective Communication: Clear, jargon-free communication is essential. Providers should explain the risks and benefits of different options in a way that is understandable to the patient.
- Understanding Patient Values: Providers should actively listen to patients to understand their values, preferences, and lifestyle considerations.
- Presenting Evidence-Based Options: Clinicians must present all reasonable options, supported by the latest evidence, allowing patients to make informed choices.
- Decision Aids: Tools such as pamphlets, videos, and interactive websites can facilitate the decision-making process by providing structured information.

Common Pitfalls and Solutions
While shared decision-making offers numerous benefits, there are challenges to its implementation:
- Misinformation: The abundance of inaccurate health information online can influence patient decisions. Providers need to address misinformation directly and provide reliable sources.
- Time Constraints: In busy clinical settings, time can be a limiting factor. Efficient use of decision aids and pre-visit planning can help mitigate this issue.
- Varying Health Literacy: Patients have different levels of understanding regarding medical information. Tailoring communication strategies to meet individual literacy levels is crucial.
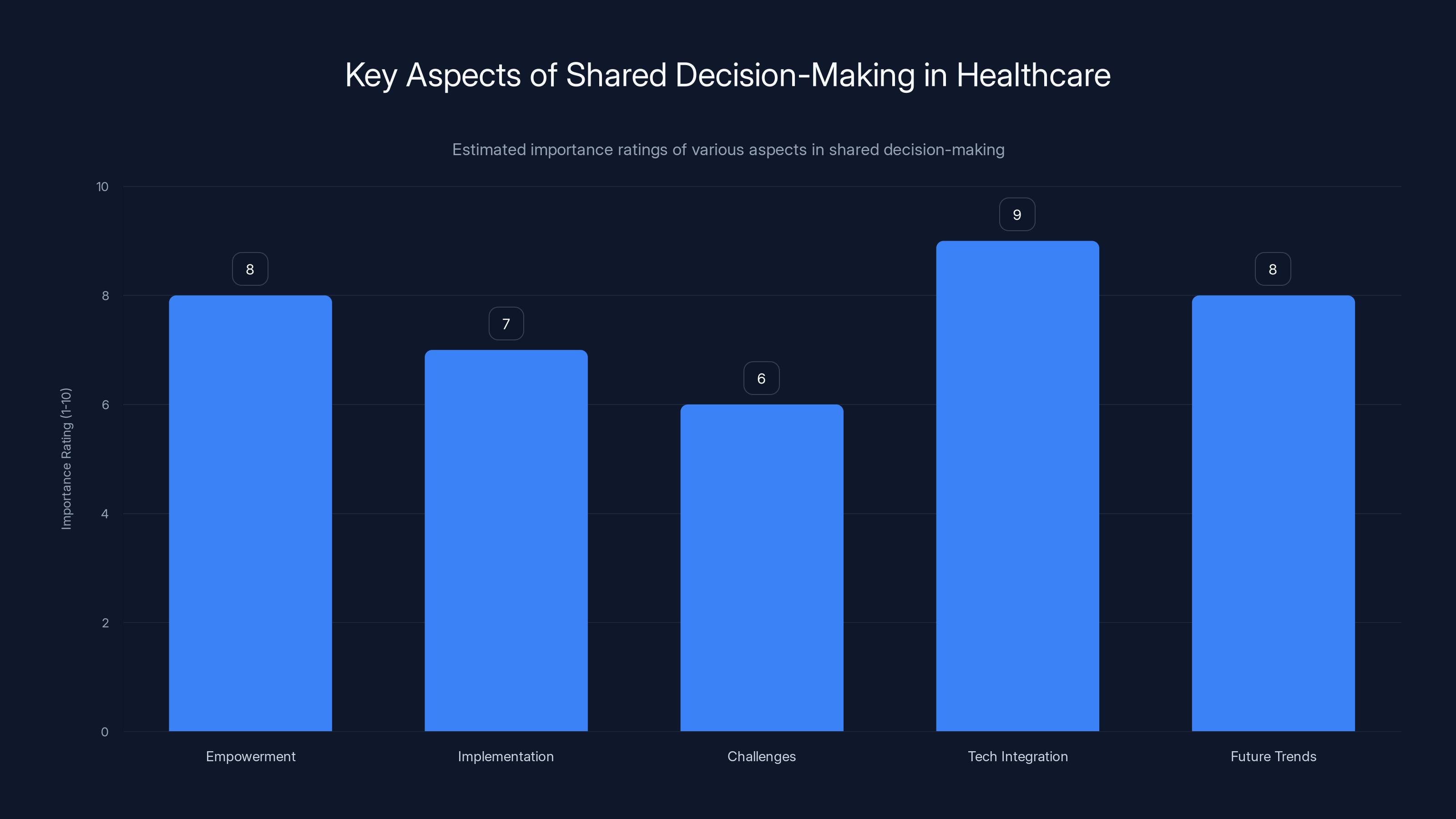
Technological integration and empowerment are highly rated aspects, indicating their crucial role in shared decision-making. Estimated data.
Technological Integration in Shared Decision-Making
Technology can play a significant role in enhancing shared decision-making processes. Digital tools and platforms can provide patients with access to personalized health information and support informed decision-making.
AI-Powered Tools
AI-driven applications can analyze patient data to generate tailored recommendations, helping patients understand potential outcomes and make informed choices.
Telemedicine and Remote Consultations
The rise of telemedicine has expanded opportunities for shared decision-making by allowing patients to engage with healthcare providers from the comfort of their homes. This accessibility can lead to more frequent and meaningful interactions between patients and providers.

Future Trends and Recommendations
The future of shared decision-making in vaccine policy and healthcare, in general, is promising. Here are some anticipated trends and recommendations:
- Wider Adoption: As more healthcare systems recognize the benefits of patient-centered care, shared decision-making is likely to become a standard practice.
- Policy Adjustments: Government agencies and healthcare organizations may develop policies that support and incentivize shared decision-making practices.
- Increased Role of Technology: Continued advancements in technology, particularly AI and digital health platforms, will further integrate shared decision-making into everyday healthcare.

Case Study: Implementing Shared Decision-Making in a Pediatric Clinic
A pediatric clinic in California implemented a shared decision-making model for vaccine consultations. By using interactive decision aids and personalized consultations, the clinic reported a 15% increase in vaccination rates and improved patient satisfaction scores.
Steps Taken
- Training Staff: All clinical staff received training on shared decision-making principles and communication techniques.
- Utilizing Decision Aids: The clinic developed digital and print materials to support vaccine discussions.
- Personalized Consultations: Each patient received a tailored consultation based on their medical history and preferences.

Conclusion
Shared decision-making represents a significant shift in healthcare, emphasizing the importance of patient autonomy and personalized care. While challenges exist, the integration of technology and continued policy support can help overcome these obstacles. As shared decision-making becomes more prevalent, it has the potential to transform vaccine policy and healthcare delivery, ultimately leading to improved health outcomes and patient satisfaction.
FAQ
What is shared decision-making in healthcare?
Shared decision-making is a collaborative process where healthcare providers and patients work together to make healthcare decisions, considering both clinical evidence and patient preferences.
How does shared decision-making benefit patients?
It empowers patients by involving them in their healthcare decisions, leading to increased satisfaction and better adherence to treatment plans.
What are the challenges of implementing shared decision-making?
Challenges include misinformation, time constraints in clinical settings, and varying levels of patient health literacy.
How can technology support shared decision-making?
Technology, such as AI tools and telemedicine platforms, can provide personalized health information and facilitate communication between patients and providers.
What is the future of shared decision-making in healthcare?
The future includes wider adoption in healthcare systems, policy support, and increased integration of technology to enhance patient-provider interactions.

Key Takeaways
- Shared decision-making involves collaborative healthcare decisions between providers and patients.
- It emphasizes patient autonomy and personalized care, leading to better health outcomes.
- Implementation challenges include misinformation and time constraints in clinical settings.
- Technological tools like AI and telemedicine enhance shared decision-making processes.
- Future trends include wider adoption and policy support for shared decision-making.
Related Articles
- Unmasking Sleep Apnea in Women: Understanding, Detecting, and Treating the Silent Epidemic [2025]
- Exploring Lenovo’s AI-Driven Robot Arm Concept with Puppy Dog Eyes [2025]
- CDC Leadership Crisis: The Ongoing Instability Threatening Public Health [2025]
- OpenEvidence's $12B Valuation: Why AI Medical Data Matters [2026]
- ChatGPT in Healthcare: 40M Daily Users & AI's Medical Impact [2025]
![The Shift Towards Shared Decision-Making in Vaccine Policy: A Comprehensive Guide [2025]](https://tryrunable.com/blog/the-shift-towards-shared-decision-making-in-vaccine-policy-a/image-1-1773050658292.jpg)



